
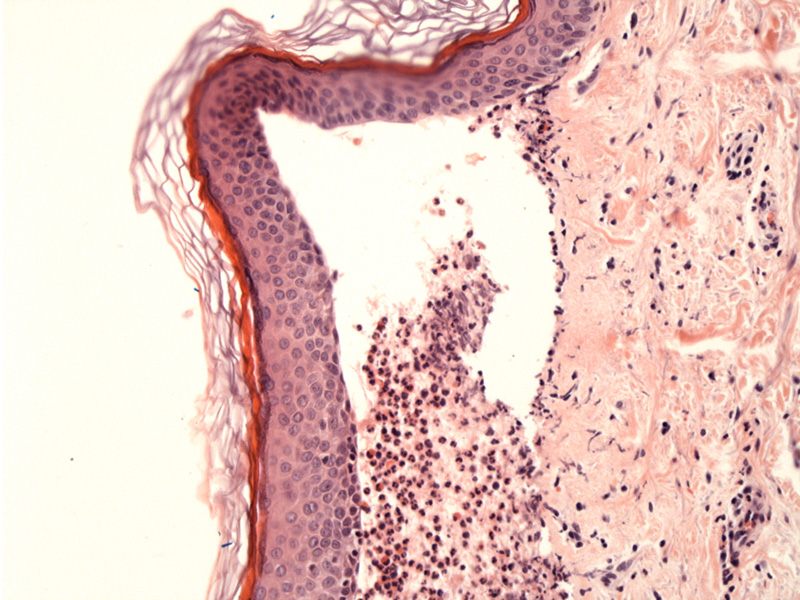
Case 1: A subepidermal vesicle (split between the epidermis and superfical dermis) is seen. Perivascular inflammation is also common.
A microabscesses (collections of neutrophils and eosinophils) is seen in the edematous dermal papillae. Other histologic features seen in bullous pemphigoid include eosinophilic spongiosis and perivascular lymphocytes and eosinophils.
Case 2: Yet another case nicely demonstrating the subepidermal clefting.
Note the prominent eosinophils, a feature of this tumor.
Bullous pemphigoid is an autoimmune blistering disease that generally affects the elderly.
In contrast to pemphigus vulgaris with IgG autoantibodies directed to desmoglein 1 and desmoglein 3 where there is loss of adhesion between keratinocytes, in bullous pemphigoid, the IgG autoantibodies are directed toward the BP1 or BP2 antigen in the basement membrane. Specifically, BP1 and BP2 antigens are components in type XVII collagen, present in hemidesmosomes of the basement membrane. Thus, the clefting in bullous pemphigoid is subepidermal (versus intraepidermal in pemphigus vulgaris).
A subtype of bullous pemphigoid is pemphigoid gestationis, also known as herpes pemphigoid (a misnomer since this is not related to the herpes virus). In pemphigoid gestationis, antibodies are also directed to the BP2 antigen leading to the formation of vesicles and bullae in the second and third trimesters of pregnancy (Rapini).
Crops of tense fluid-filled bullae arise in otherwise normal appearing skin, and are usually quite itchy. In severe cases, blisters cover the skin as well as the mouth.
Steroids.
Untreated, bullous pemphigoid often for months or years, but with treatment, most patients undergo remission 1-5 years. It may actually be lethal in highly debilitated individuals.
• Epidermis : Dermatitis Herpetiformis
Rapini RP.Practical Dermatopathology. Philadelphia, PA: Elsevier; 2005: 91-2.
DermNet NZ. Bullous pemphigoid. www.dermnetnz.org/immune/pemphigoid.html
