
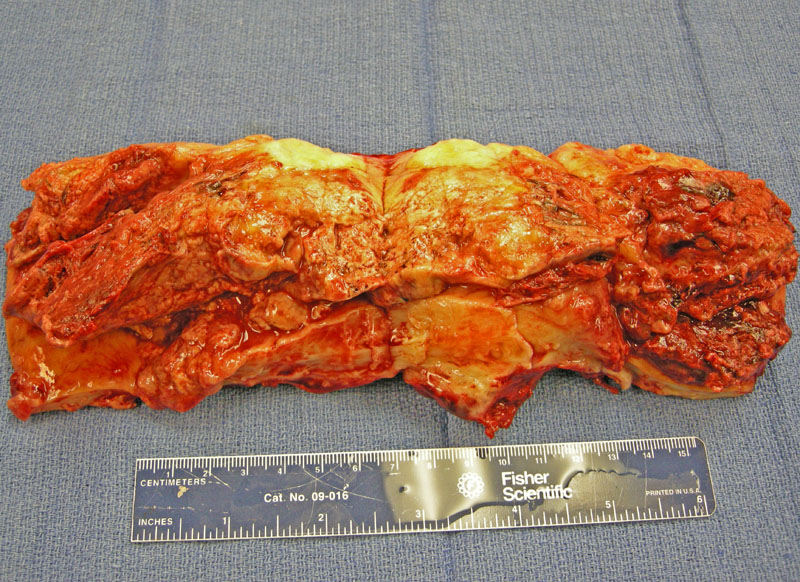
Extensive fibrin deposition of the placenta is evident grossly, the extent of which requires gross assessment in order to make a definitive diagnosis.
Replacement of the parenchyma by pale tan fibrinous material is seen.
This is one reprentative area showing the villi engulfed by widespread fibrin deposition. Most of the placenta showed areas such as this.
A different case shows similar findings grossly and microscopically, with much of the placenta consisting of fibrin.
Maternal floor infarction and massive perivillous fibrin deposition are poorly understood placental lesions reported to be associated with intrauterine growth retardation and recurrence. However, the diagnosis and classification of this entity, vs normal or massive perivillous fibrin deposition, is highly subjective and clearly fraught with problems. One accepted definitional standard put forth is as follows: massive perivillous fibrin deposition= perivillous fibrin deposition involving 30% or more of chorionic villi in central (nonbasal) region of the placenta, while maternal floor infarction = perivillous fibrin deposition involving more than 50% of basal villi associated with hypovascular or fibrotic villi.
Maternal floor infarction and massive perivillous fibrin deposition vasculopathy have been associated with recurrent adverse fetal outcomes and with maternal thrombophilia. Therefore, a diagnosis of one of these should prompt evaluation for maternal thrmbophilia, which most often proves to be protein S related.
In a study using semiquantitative histologic criteria for massive perivillous fibrin deposition and maternal floor infarction, IUGR was identified in no case with classic maternal floor infarctoin, in 31% of cases with transmural or borderline massive perivillous fibrin deposition, and in 11% of cases with neither lesion. Recurrence was seen in 1 of 7 (14%) second- or third-trimester placentas, while possible recurrence was suggested in 3 of 6 (50%) first-trimester spontaneous abortion cases. Classification of intraplacental fibrin is subjective and problematic; almost half of potential cases of MFI or MFD did not fulfill our study's diagnostic criteria. MFD may be more common and more strongly associated with IUGR than classic MFI. Recurrence of these lesions appears to be infrequent among second- and third-trimester placentas, but may be relatively common in first-trimester spontaneous abortions.
Katzman PJ, Genest DR.Maternal floor infarction and massive perivillous fibrin deposition: histological definitions, association with intrauterine fetal growth restriction, and risk of recurrence. Pediatr Dev Pathol. 2002 Mar-Apr;5(2):159-64.
Chen-Chih J. Sun, et al. Discrepancy in Pathologic Diagnosis of Placental Lesions. Archives Pathol Lab Med: Vol. 126, No. 6, pp. 706–709.
Gogia N, Machin GA. Maternal thrombophilias are associated with specific placental lesions.
Pediatr Dev Pathol. 2008 Nov-Dec;11(6):424-9.