
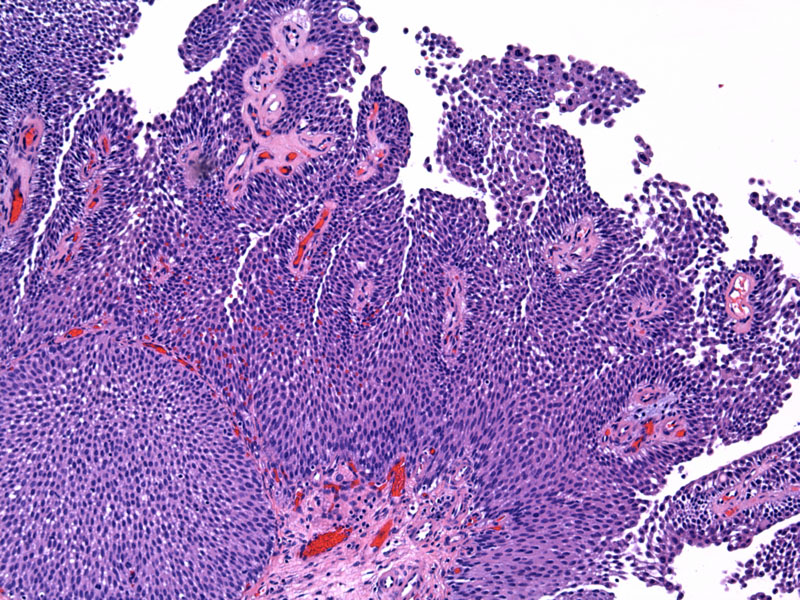
Papillary urothelial neoplasm of low malignant potential (PUNLMP) have well-developed papillary structures lined by cytologically bland cells. There is an increased urothelial cell layer.
The papillary structures are lined by urothelium devoid of atypia. There is no increase in the thickness of the epithelium. The cytomorphology and arrangement of the cells resembles normal urothelium except for the papillary nature of the growth. Note that some may called this a 'papilloma' instead of a PUNLMP. Read the background information for more discussion.
Here is the classification scheme proposed by the WHO in 2004.
Histological features of Papillary Urothelial Lesions, adapted from reference 3.
Papillary urothelial neoplasm of low malignant potential (PUNLMP) has long and tortuous history. In 1973, the WHO grading scheme for papillary urothelial neoplasms contained 4 categories: urothelial papilloma (benign) and papillary urothelial carcinoma grades 1-3. However, some pathologists wanted to avoid the label of "carcinoma" for grade 1 lesions that essentially behaved in an indolent and mostly benign fashion. PUNLMP was created as a category for these tumors with very low-grade histologic features, but were more cellular than a papilloma. To further complicate the picture, noninvasive lesions of this organ (bladder, ureter and urethra) are historically term 'carcinoma'. Therefore, the reasoning being PUNLMP seems rather patchy, considering low grade or high grade papillary urothelial carcinomas are not true carcinomas with invasion.
There are some pathologists that simply deny the existence of PUNLMPs, maintaining that the term is not well-defined and many PUNLMPs are actually low-grade carcinomas. Supporting this assertion is the fact that followup of PUNLMPS demonstrate similar recurrence and progression rates as low-grade papillary urothelial carcinomas.
In anycase, the debate continues and the current 2004 WHO/ISUP classification is as follows:
- Papilloma: Normal urothelial lining a fibrovascular core. The epithelium has the normal thickness with well-organized and polarized cell. There is no mitoses. These lesions are small, isolated and rare, found in younger patients.
- PUNLMP: These lesions look larger and thicker than papillomas, but there is no (or minimal) cytologic atypia. There are increased cell layers, but the cells are still well-organized, polarized with normal or slightly increased N/C ratios. Mitoses are very rare, and located only at the basal layer.
- Low grade papillary urothelial carcinoma: Urothelial lining is thickened with moderate organization (mostly polarized). There is mild cytologic atypia and occasional mitoses.
- High-grade papillary urothelial carcinoma: Disordered urothelium with a lack of polarity and orientation. The cells should look similar to CIS with marked cytologic atypia (pleomorphism, hyperchromasia, prominent nucleoli) and frequent mitotic figures.
Note that according to the WHO definition, a thickened cell layer is not a requirement of PUNLMP or low-grade/high-grade carcinomas. However, if a thickened cell layer is not needed to diagnosis a PUNLMP and this entity has no (or very minimal) atypia, then features to distinguish PUNLMP from a papilloma is not clear. Anyone who may know this answer is encouraged to send us an email.
Common symptoms are gross or microscopic hematuria.
The variable fate of PUNLMPs is what creates the controversy. In general, a certain subset of PUNLMPS recur, and of those that recur, a significant percentage recur as a low-grade carcinoma with a smaller percentage progressing to invasive carcinoma. In a 112 series of PUNLMP cases, tumor recurrence occurred in 29%, and of these recurrent cases, 75% had a higher-grade tumor. In another study of 322 PUNLMP cases, they found no difference between tumor recurrence and progression to high-grade lesions between PUNLMP and low-grade carcinoma cases.1
Thus, suffice to say that the grading of papillary urothelial lesions is still evolving and another classification may arise as new discoveries (ie. genetics) help us predict the behavior of seemingly benign papillary lesions.
• Bladder : Transitional Cell Carcinoma, Low Grade
• Bladder : Transitional Cell Carcinoma, High Grade (Invasive)
1 Jones TD, Cheng L. Papillary Urothelial Neoplasm of Low Malignant Potential: Evolving Terminology and Concepts. The Journal of Urology. 2006;175:1995-2003.
2 Lopez-Beltran, A. Bladder cancer: Clinical and pathological profile. Scandinavian Journal of Urology and Nephrology. 2008;42(Suppl218):95-109.
3 Rodolfo Montironi and Antonio Lopez-Beltran. The 2004 WHO Classification of Bladder Tumors: A Summary and Commentary. Int J Surg Pathol 2005; 13; 143