
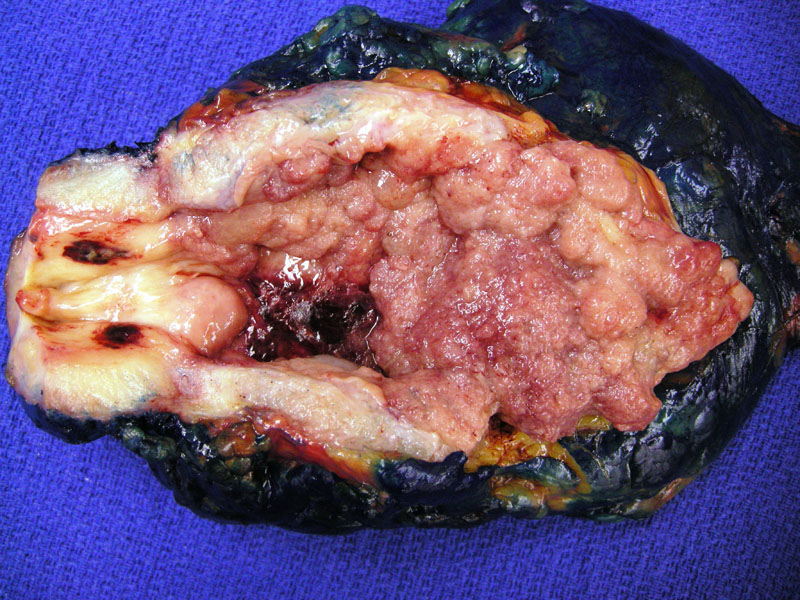
An exophytic papillary friable transitional cell carcinoma is filling the lumen of the bladder.
Bladder surface shows high grade papillary carcinoma.
Disordered growth of broad cords of infiltrating transitional cell carcinoma into the muscularis is appreciated.
Although invasion of the lamina propria yields a worse prognosis, the most significant decrease in survival is associated with tumor invading the muscularis propria, as demonstrated here.
Urine cytology shows increased cellularity composed of groups of neoplastic transitional cells as well as many single cells. Sometimes increased cellularity is not seen in the urine, in cases of TCC.
The cells show pronounced cytological atypia including clumped chromatin, pleomorphism, cellular enlargement and a high nuclear:cytoplasmic ration. Nucleoli, a feature of high grade tumors, are also appreciated.
Another case shows high grade papillary TCC along the surface with extensive lamina propria involvement. The cells take on an eosinophilic cytoplasmic quality upon invasion, a feature helpful in cases of only focal limited microinvasion. This tumor actually showed muscularis propria involvement as well.
High grade TCC can show neural involvement. Malignant cells surrounding and within this nerve are seen.
Rarely a high grade transitional carcinoma shows sarcomatoid differentiation. This image shows high grade spindle cells, but examples of osteosarcoma or other specific sarcomas may also arise.
For high grade papillary carcinoma, the progression rate to invasive carcinoma ranges from 15% to 40%.1 Some textbooks (Robbins) even quote numbers as high as 80%.2 Heterogeneity of grade is recognized in papillary lesions and the consensus is that tumors should be graded on their most atypical part (although this assertion still needs further study). The presence of disorganization among the cells and nuclear pleomorphism are key features for diagnosing a tumor as high grade. Nucleoli are often apparent and may be prominent. High grade tumors often show apparent solid masses due to fusion of papillae.
Invasion of muscularis propria has important prognostic implications, as it results in a 5-year survival rate of 50%.2 As a side note, it is important to realize that in some people, the bladder contains a muscularis muscosa, which may be form a continous band in the lamina propria or appear as discontinuous dabs of muscle.3 The pathologist must not confuse involvement of the more superficial muscularisa mucosa with the deeper muscularis propria (detrusor muscle), and thus, upstage the patient erroneously.
These tumors, when noninvasive (pTa), likely all require resection of tumor +/- intravesical therapy such as immunotherpay with BCG. Higher stage lesions require more extensive surgery such as cystectomy.
• Bladder : Transitional Cell Carcinoma, High Grade (Invasive)
1 Zhou M, Magi-Galluzzi, C. Genitourinary Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elvesier; 2006: 172-8.
2 Kumar V, Abbas AK, Fausto N. Robbins and Cotran Pathologic Basis of Disease. 7th Ed. Philadelphia, PA: Elsevier; 2005: 1028-1033.
3 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 532.