
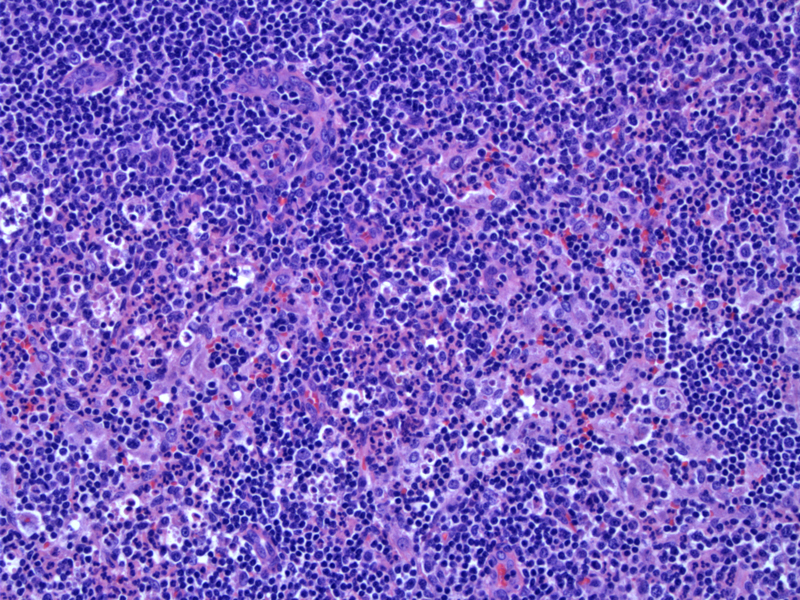
An early lesion with only scant cellular debris, some monocytoid cells and scattered neutrophils is seen. The nodal response is characterized first by follicular hyperplasia and hyperplasia of the so-called
A later stage is seen, with a fully developed granuloma with a central necrotizing center and pallisading histiocytes.
Yet another image of a characteristic granuloma with central necrosis and peripheral palisading histiocytes. The granulomas are sometimes described as stellate, but this granuloma is more round.
Cat Scratch lymphadenitis is caused by the gram-negative bacterium Bartonella henselae. It is found in feline red cells and fleas, which can contaminate saliva and be introduced into humans through biting and clawing by cats. The organism has a worldwide distribution and in northern temperate zones, it occurs more often in August through October, usually in humid, warm locales.
This species is quite difficult to culture, which is therefore not routinely recommended. Serology is the best initial mode for diagnosis and can be performed by indirect fluorescent assay or enzyme-linked immunosorbent assay. Serology lacks specificity because many asymptomatic persons have positive results from previous (often asymptomatic) exposure.
Initially, there is follicular hyperplasia with monocytoid B-cell hyperplasia around the follicles and within sinuses. Aggregates of neutrophils and histiocytes forming microabscesses are seen. In later stages, well-developed stellate granulomas with peripheral pallisading histiocytes and central area of necrosis are characteristic.
If a Warthin-Starry stain is performed, the coccobacilli can be found in the areas of necrosis or within endothelial cells or histiocytes.
Affected patients are usually children or young adults although any age can be afflicted. Presentation includes a papule (at the site of entry) and within 1-2 weeks, regional lymphadenopathy develops which is usually tender. Occasionally, the inflammation can extend through the lymph node capsule and form a fistula with overlying skin. The majority develop aches, malaise, and depressed appetite, and a small percentage develop low-grade fever.
Lymphadenopathy may remain for months. Visceral involvement has been reported but is uncommon. A skin test is positive in 90% of cases (Weiss).
In immunosuppressed patients, B. henselae can cause bacillary angiomatosis and peliosis.
Treatment should be based on the disease presentation. Most patients, especially children, have self-limited lymphadenopathy lasting two to eight weeks and thus do not require antibiotic therapy. For the small percentage that develop dissemination to the liver, spleen, eye, or central nervous system and antibiotics may be of use.
Treatment of bacillary angiomatosis and peliosis involves erythromycin or doxycycline for a prolonged course of several months.
In most cases, the disease is self-limited. Rare complications include encephalitis and neuroretinitis.
Cat scratch should be considered in the differential diagnosis of fever of unknown origin and any lymphadenopathy syndrome.
Asymptomatic, bacteremic cats with Bartonella henselae in their saliva are potential vectors and cat fleas are responsible for horizontal transmission from cat to cat.
Most patients have a self-limited course, especially children.
Weiss L. Lymph nodes: Illustrated Surgical Pathology New York, NY: Cambridge University Press; 2008: 71-2.
