
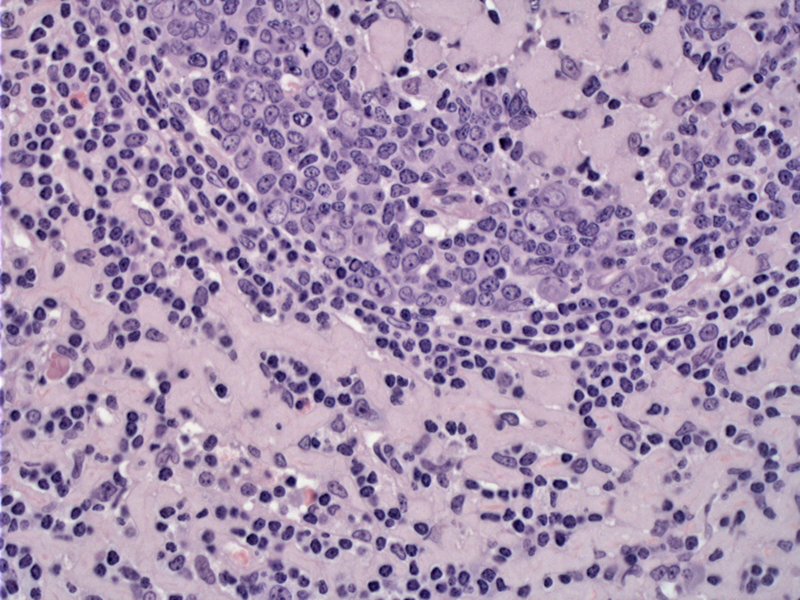
Amyloid infiltrates and isolates small numbers of lymphocytes in this node. While not seen here, typically amyloid also deposits around the vessel walls, . Foreign body giant cells and plasma cells may be seen in the milieu.
Case 1 - The germinal center is largely replaced by amyloid, as well as areas in the interfollicular zone. The amyloid is quite waxy appearing.
Case 2 - More advanced involvement is seen. There is little lymphoid material left.
Amyloid deposition in a lymph node can occur as a result of neoplasia (e.g. plasma cell dyscrasia, Non-Hodgkin's lymphoma) or in association with systemic or localized amyloidosis. Amyloid deposits in the lymph node are found in 1/3 of patients with systemic amyloidosis at autopsy and in 22% of uremic patients (O'Malley).
There are several types of amyloid, namely AA and AL types. In patients with primary amyloidosis, the AL type is found, whereas in those with inflammation or infections, it is the AA type. Occasionally, beta-2-microglobuin associated amyloid may be seen in patients with uremia underlying hemodialysis.
Grossly, partial involvement of the spleen or lymph node consists of amyloid in the white pulp and is described as "sago" spleen. Sago pearls are tapioca-like. When there is diffuse amyloid, the spleen or lymph node looks waxy and is called "lardaceous".
For AL amyloidosis manifesting as lymphadenopathy, the prognosis is usually good if there are no hematological malignancies or any rapid increase in the size of lymph nodes. Many cases show shrinkage in node size following chemotherapy. For cases of the systemic amyloid type, more intensive chemotherapy should be considered to address possible involvement of visceral organs.
• Spleen : Splenic Amyloidosis
• Oral Cavity : Amyloidosis (Tongue)
O'Malley DP et al. Benign and Reactive Conditions of Lymph Node and Spleen: Atlas of Nontumor Pathology First Series, Fascicle 7. Washington DC; AFIP: 2009: 445-7.