
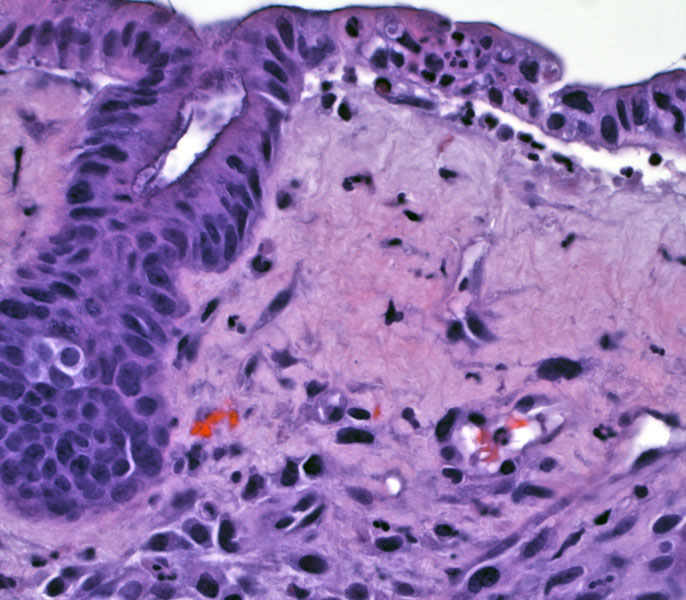
Acute ischemia damages the superficial portion of the colonic mucosa while the deeper portion of the crypts are spared. In this image, the surface epithelium is damaged and frayed, and overlies a fibrotic lamina propria. Note that a smudgy and hyalinized lamina propria is highly characteristic of ischemic colitis.
There is marked glandular dropout and simplification (glandular cells lose their mucin and have a flattened appearance). Note again the hyalinized lamina propria. Hemorrhage within the lamina propria is also another common feature.
Depending on the severity of the ischemia and its duration, ischemic colitis can have a wide range of clinical presentation and morphology. It can range from mild chronic ischemic changes limited to the mucosa, to transmural infarction of the bowel leading to gangrene. In this case, we are demonstrating acute ischemic colitis limited to the mucosa.
Generally occurs in patients over 50 with predisposing conditions such as atherosclerosis and diabetes. However, the condition can also occur younger patients in association with collagen vascular diseases (due to vasculitis), hypovolemia and as a rare complication of birth control pills (possibly due to prothrombotic effects of estrogen).1,2 Basically, any condition that causes decreased blood flow to the colon can lead to ischemic colitis.
Grossly, there may be ulceration, psuedomembranes and marked edema of the mucosa. A chronice or healed ischemic segment may form strictures and have similar endoscopic appearance as Crohn's disease.1,3
Treat underlying condition. Surgery may be necessary to remove injured or infarcted bowel.
1 Odze RD, Goldblum JR, Crawford, JM. Surgical Pathology of the GI Tract, Liver, Biliary Tract, and Pancreas. Philadelphia, PA: Elsevier; 2004:232-4.
2 Rosai, J. Rosai and Ackerman's Surgical Pathology. 9th Ed. Philadelphia, PA: Elsevier; 2004:790-1.
3 Iacobuzio-Donahue CA, Montgomery EA. Gastrointestinal and Liver Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier; 2005:331-3.