
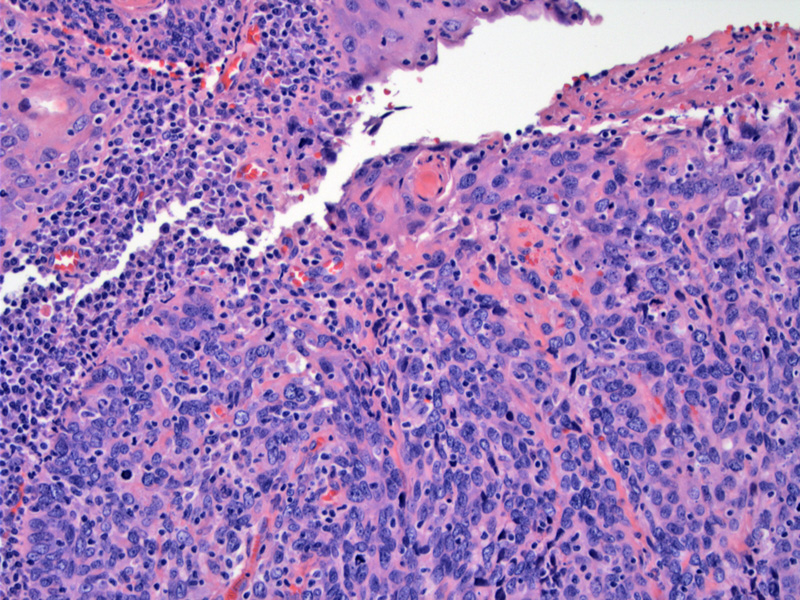
The surface of the tumor is eroded, with an overlying fibrinous exudate seen to the upper right. There mucosa is replaced by hyperchromatic large cells.
The surface shows high grade dysplasia, with enlarged dark cells crowded tightly together. There is mucosal inflammation as well.
The normal tonsil is comprised of mature lymphocytes, and is involved by cohesive nests of malignant cells that are hard to identify as squamous.
The squamous cell carcinoma is poorly differentiated, although a few cells contain cytoplasm hinting as to its keratinizing nature.
Strong p16 staining is seen in this tumor, and appropriately lacking in the lymphoid tonsillar tissue for comparison.
The orophayrnx is the middle portion of the pharynx, composed of multiple subsites:
- Base of the tongue, which includes the pharyngoepiglottic folds and the glossoepiglottic folds.
- Tonsillar region, including the palatine tonsils, tonsillar fossae and the anterior and posterior pillars.
- Anterior surface of the soft palate, including the uvula
- Pharyngeal walls including the posterior and lateral surfaces.
Tobacco and alcohol abuse are the most significant risk factors for oropharyngeal cancer. Increasingly, infection with the human papillomavirus (HPV)(especially HPV-16) is seen in association with this malignancy.
Base of tongue cancers typically grow in either an infiltrative or exophytic pattern. Due to relatively few afferent nerve fibers in this region, base of tongue lesions can remain somewhat asymptomatic until they enlarge significantly. When common late symptoms include dysphagia, weight loss, referred otalgia due to CN IX involvement, trismus from pterygoid muscle invasion, tongue immobility from aterior extension into the deep tongu musculature and a mass in the neck (>70% of affected patients have ipsilateral cervical nodal metastases to levels II and III).
Withing the tonsillar region,the anterior tonsillar pillar and tonsil are the most common location for a primary tumors. Syptoms are similar to those of the base of tongue and malignancies can grow into adjacent regions including the lateral soft palate, retromolar trigone and buccal mucosa, and deep tonsillar fossa. Here again, the lymphatic drainage is primarily to level II nodes.
Pharyngeal wall malignancies are also typically diagnosed in an advanced stage because of their location and patient compensation and denial. These cancers can extend superiorly to the nasopharynx, posteriorly to the prevertebral fascia, and inferiorly to involve the hypopharynx. Primary lymphatic drainage is to the retropharyngeal nodes and level II and III nodes, and bilateral cervical metastases are seen more commonly than more lateral oropharyngeal subsites.
Recognition of the role of HPV in oropharyngeal cancer is evolving. Individuals with HPV16 oral infection have a 14 times increased risk of developing HPV+ oropharyngeal cancer2 . The extent of synergistic carcinogenesis between HPV-16 and tobacco/EtOH is unclear, although HPV infection in the basal mucosal epithelium is recognized as the most common risk factor in individuals without a history of tobacco/EtOH use3 . HPV associated cancers are thought to be related to viral E6 and E7 proteins that inactivate p53 and retinoblastoma protein respectively, causing to malignant transformation of HPV infected cells. Risk factors for HPV associated oropharyngeal cancer are high number of sexual partners4 (25% increase >= 6 partners6 ), history of oral-genital sex6 (125% greater risk with >= 4 partners5 ), history of anal–oral sex4 , female partner with a history of either an abnormal Pap smear or cervical dysplasia7 , frequent marijuana use8 and, among men, decreasing age at first intercourse and history of genital warts4 .
Treatment for oropharyngeal cancer is typically multi-modality based, especially for higher steged cases. For small and limited disease surgery with radiation or radiation therapy alone has been used to minimize morbidity. For mid to higher staged disease, surgery followed by radiation therapy or chemo/radiation therapy is the mainstay of treatment. The role of cetuximab, a monoclonal antibody to an epidermal growth factor receptor, in HPV+ disease has shown promising results10 . Despite surgical advances in resection and reconstruction in the past 15 years, non-surgical treatment has escalated morbidity in affected patients, often causing lifelong xerostomia and dysphagia.
HPV associated disease is seen to have a better therapeutic response and survival compared with HPV-negative malignancies9 . Generally accepted statistics show an 80–95% 2-3 year survival rate for the HPV+ cases and 57–62% for the HPV- disease11
• Oral Cavity : Necrotizing sialometaplasia
• Thyroid : Anaplastic Carcinoma, Squamoid Type
1. http://www.cancer.gov/cancertopics/pdq/treatment/oropharyngeal accessed 2/21/2010.
2. Michl, P; Pazdera, J; Prochazka, M; Pink, R; Stosova, T (2010). "Human papillomavirus in the etiology of head and neck carcinomas" (PDF). Biomedical papers of the Medical Faculty of the University Palacky, Olomouc, Czechoslovakia 154 (1): 9–12. PMID 20445705
3. Mannarini, L; Kratochvil, V; Calabrese, L; Gomes Silva, L; Morbini, P; Betka, J; Benazzo, M (2009). "Human Papilloma Virus (HPV) in head and neck region: review of literature". Acta otorhinolaryngologica Italica : organo ufficiale della Societa italiana di otorinolaringologia e chirurgia cervico-facciale 29 (3): 119–26. PMID 20140157
4. Schwartz, SM; Daling, JR; Doody, DR; Wipf, GC; Carter, JJ; Madeleine, MM; Mao, EJ; Fitzgibbons, ED et al. (1998). "Oral cancer risk in relation to sexual history and evidence of human papillomavirus infection". Journal of the National Cancer Institute 90 (21): 1626–36. PMID 9811312
5. Heck, J.; Berthiller, J.; Vaccarella, S.; Winn, D.; Smith, E.; Shan'gina, O.; Schwartz, S.; Purdue, M. et al. (2009). "Sexual behaviours and the risk of head and neck cancers: a pooled analysis in the International Head and Neck Cancer Epidemiology (INHANCE) consortium". International journal of epidemiology 39 (1): 166–181. doi:10.1093/ije/dyp350. PMID 20022926
6. Smith, E.; Ritchie, J.; Summersgill, K.; Klussmann, J.; Lee, J.; Wang, D.; Haugen, T.; Turek, L. (Feb 2004). "Age, sexual behavior and human papillomavirus infection in oral cavity and oropharyngeal cancers". International journal of cancer. Journal international du cancer 108 (5): 766–772. PMID 14696105
7. Hemminki, K; Dong, C; Frisch, M (Dec 2000). "Tonsillar and other upper aerodigestive tract cancers among cervical cancer patients and their husbands". European journal of cancer prevention : the official journal of the European Cancer Prevention Organisation (ECP) 9 (6): 433–7. PMID 11201683
8. Gillison, M.; D'souza, G.; Westra, W.; Sugar, E.; Xiao, W.; Begum, S.; Viscidi, R. (Mar 2008). "Distinct risk factor profiles for human papillomavirus type 16-positive and human papillomavirus type 16-negative head and neck cancers" (Free full text). Journal of the National Cancer Institute 100 (6): 407–420. PMID 18334711
9. Ang, K. K.; Harris, J.; Wheeler, R.; Weber, R.; Rosenthal, D. I.; Nguyen-Tan, P. F.; Westra, W. H.; Chung, C. H. et al. (2010). "Human Papillomavirus and Survival of Patients with Oropharyngeal Cancer". New England Journal of Medicine 363 (1): 24. doi:10.1056/NEJMoa0912217. PMID 20530316
10. Eriksen, J. G.; Lassen, P.; Overgaard, J. (2010). "Do all patients with head and neck cancer benefit from radiotherapy and concurrent cetuximab?". The Lancet Oncology 11 (4): 312. doi:10.1016/S1470-2045(10)70035-8. PMID 20359659
11. Fakhry C, Westra WH, Li S, et al. Improved survival of patients with human papillomavirus-positive head and neck squamous cell carcinoma in a prospective clinical trial. Journal of the National Cancer Institute. 2008;100(4):261–269.