
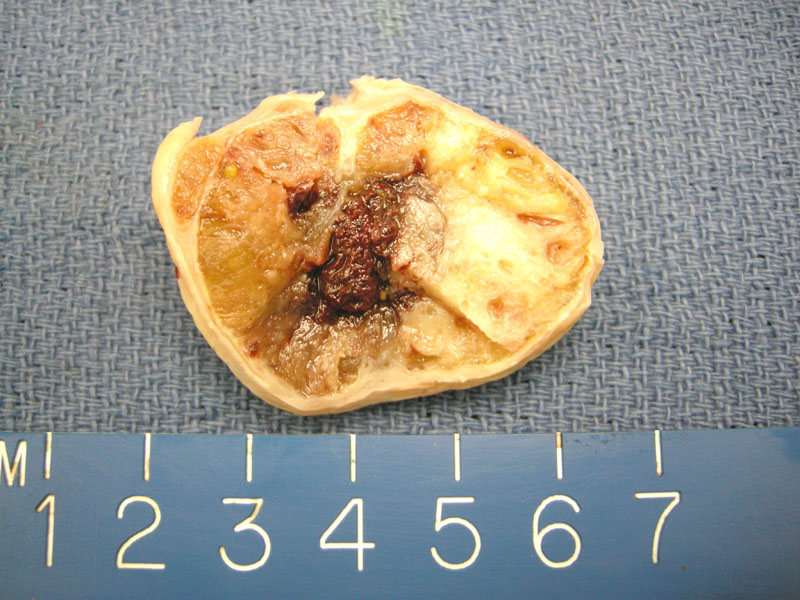
The gross impression of the ovarian tumor often provides a clue to its constituents, as this one shows tan glistening parenchyma with intervening fibrosis. When arising in the ovary, this appearance is highly suggestive of struma ovarii.
Another perhaps less obvious example shows a yellow tan glistening 970gm tumor with cystic and hemorrhagic change.
The criteria for a diagnosis of struma ovarii requires that the thyroid tissue comprise at least 50% of the tumor. This case demonstrated numerous thyroid follicles filled with colloid.
Struma ovarii can exhibit the full spectrum of morphologies seen in the thyroid gland, ranging from mature normal thyroid tissue to hyperplasia, adenomas and carcinomas (most commonly papillary thyroid carcinoma, although follicular can be seen as well). This image demonstrates dilated follicles filled with colloid, similar to those seen in a multinodular goiter.
A prominent lymphocytic infiltrate, commonly seen in the thyroid, can also be seen in the ovarian stroma. Although not demonstrated in this case, luteinization of ovarian stromal cells at the periphery of the stroma ovarii is often present.
Struma ovarii is the most common monodermal teratoma (a mature teratoma composed of tissues derived from a single germ cell layer). The latin term for a goiter is struma, therefore, struma ovarii literally translates to a goiter of the ovary. Other less common monodermal teratomas include carcinoids and neuroectodermal tumors.
Although thyroid tissue can be found in up to 15% of teratomas, the diagnosis of struma ovarii requires that the lesion must consist of 50% or more of the thyroid tissue. Thus, struma ovarii is quite rare and represents 1-3% of all benign ovarian teratomas.1,2
Peak incidence is in the 5th decade, and most patients are asymptomatic. However, some patients may present with a pelvic mass, ascites, and rarely Meigs syndrome (clinical triad of right-sided pleural effusion, ascites, and classically an ovarian fibroma). Hyperthyroidism occurs in about 5% of patients.4
These tumors have an excellent prognosis, even if extra-ovarian tumor is present. Note that the issue of malignant stroma ovarii is contentious, and its definition is still evolving. No doubt that there have been well-documented cases of metastases and extra-ovarian spread of struma ovarii, however, due to the rarity of this tumor, it has been difficult to obtain enough cases to identify features with prognostic value.
For example, many past cases of malignant stroma ovarii exhibited histology identical to thyroid carcinomas, however, these cases did not metastasize. It is not clear if the same grading and staging criteria for thyroid carcinomas can be directly applied to struma ovarii.
Robboy and colleagues (2009) conducted the largest study to date of 88 cases of malignant struma ovarii and identified features associated with a more biologically malignant tumor (defined as tumor spread onto the surface of the ovary or beyond). These features included: the size of the struma ovarii component (>12cm), presence of adhesions, ovarian serosal rent and peritoneal fluid greater 1 liter.3
In their summary discussion, Robboy surmised that no single histologic features with the possible exception of papillary carcinoma and poorly differentiated carcinoma had clear prognostic value. The study reported a 10 and 25 year survival rate of 98% and 92% for patients with adenomatous (proliferative) histology and a 10 and 25 year survival rate of 81% and 60% for those with malignant histology. The reported overall survival from this study was 89% at 10 years and 84% at 25 years.4
♥ Greater than 50% of thyroid tissue must be present before the diagnosis of struma ovarii can be made.
♥ All types of pathology found in the thyroid can be also be found in a struma ovarii.
• Ovary : Mature Cystic Teratoma
1 Nucci MR, Oliva Esther. Gynecologic Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier: 2009: 523-6.
2 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 612-3.
3 Robboy SJ, Shaco-Levy R, Peng RY et al. Malignant Struma Ovarii: An Analysis of 88 Cases Including 27 with Extraovarian Spread. International Journal of Gynecological Pathology. 2009: 28; 405-422.
4 Roth LM, Talderman A. The enigma of struma ovarii. Pathology. 2007:39(1); 139-146.