
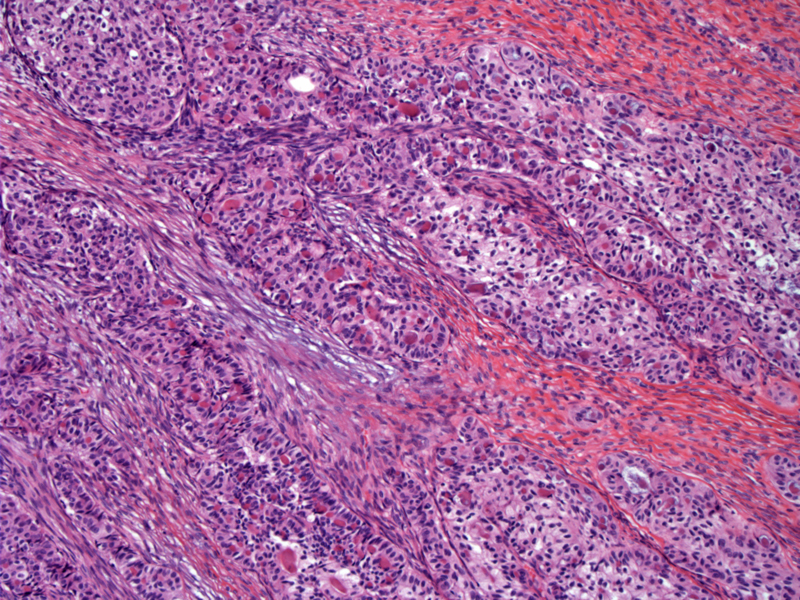
Elongated closed tubules forming broad trabeculae are a typical pattern in sertoliform endometrioid tumors.
Compact anastamosing cords are seen with some glandular differentiation. The glandular lumens contain eosinophilic secretions. This is not usually seen in Sertoli cell tumors.
The nuclear atypia of endometrioid carcinomas is often more pronounced than Sertoli cell tumors, which generally contain bland uniform nuclei in its well-differentiated form.
The reticular growth pattern is clearly seen, as well as a desmoplastic stromal response.
Several unusual variants of endometrioid adenocarcinoma exist which may mimic sex-cord stromal tumors. The microglandular pattern resembles a granulosa cell tumor; the glandular cells may even form spaces similar to Call-Exner bodies. The sertoliform pattern (discussed here) mimics Sertoli or Sertoli-Leydig tumors of the ovary, with tubular glands and formation of trabeculae.1
In most situations, the two can be distinguished from clinical, gross and histologic features. For example, Sertoli cell and Sertoli-Leydig tumors are usually unilateral. The histologic pattern generally consists of open tubules or closed tubules two or three cells thick. Trabeculae formation and diffuse growth may often be seen as well.
In contrast, endometrioid tumors may be bilateral in advanced stages and generally exhibit other growth patterns (glandular, papillary, villoglandular). The nuclei are often more atypical than Sertoli cell tumors. Glandular lumens often contain mucinous secretions (versus absent or small amounts of secretions in Sertoli cell tumors). Other helpful diagnostic features include squamous metaplasia, adjacent foci of endometriosis and areas of borderline or benign endometrioid adenofibroma.1,2
In situations when the two cannot be distinguished histologically, IHC panels will be helpful. Sex-cord tumors are generally negative for EMA and strongly positive for inhibin and calretinin. Endometrioid tumors are positive for EMA and negative for inhibin and calretinin. A recent study conducted by Zhao (2007) found that CK7, ER and PR are as helpful as EMA in distinguishing endometrioid tumors (CK+, ER+, PR+) from Sertoli cell tumors (CK-, ER-, PR-).2
Clinically, sertoliform endometrioid adenocarcinoma affects an older population (60-70 years), while Sertoli-Leydig tumors affect those of average age of 25 years and may be accompanied by endocrine manifestations (Misar).
• Ovary : Endometrioid Borderline Tumor
• Ovary : Endometrioid Adenocarcinoma
• Ovary : Sertoli-Leydig Cell Tumor
1 Mills SE, ed. Sternberg's Diagnostic Surgical Pathology.4th Ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004: 2561.
2 Zhao C, Bratthauer GL, Barner R et al. Comparative analysis of alternative and traditional immunohistochemical markers for the distinction of ovarian sertoli cell tumor from endometrioid tumors and carcinoid tumor: A study of 160 cases. Am J Surg Pathol 2007 Feb;31(2):255-66.
3 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 580-1.
4 Misir A, Sur M.Sertoliform endometrioid carcinoma of the ovary: a potential diagnostic pitfall. Arch Pathol Lab Med. 2007 Jun;131(6):979-81.