
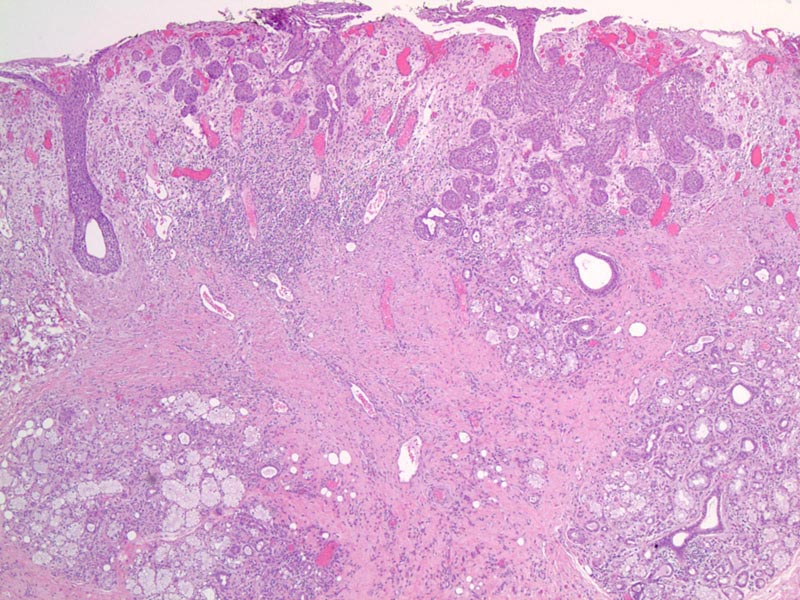
Microscopically, the key features include: (1) retained lobular configuration - an important feature distinguishing it from squamous cell carcinoma; (2) partial coagulative necrosis of salivary gland acini; (3) squamous metaplasia of excretory ducts; (4) pseudoepitheliomatous hyperplasia of overlying mucosa; (5) prominent inflammatory infiltrate.2
Squamous metaplasia of the excretory ducts is prominent.
This benign process can be discerned from squamous cell carcinoma if one examines the low power impression.
Necrotizing sialometaplasia (NS) is a reactive condition that mimics malignancy both clinically and histologically. Most cases arise spontaneously, but some patients provide a history of surgery, trauma, radiation or vomiting. Pathogenesis is generally attributed to ischemic damage to salivary glandular tissue.1
There is a wide age range (1.5 to 83 years) with an average age of 46 years. There is a male predilection (M:F ratio of 2:1). An ulcerated, crater-like lesion on the palate which develops rapidly and fails to heal is the common presentation. Pain and numbness may elicit further concerns of malignancy.2
This lesion usually occurs in the minor salivary glands (75% of cases involve the posterior palate), however, it can occur in a wide variety of locations including the parotid (8.5% of cases), submandibular and minor mucous glands of the nasopharynx, lung and trachea. Interestingly, a similar lesion is found in the breast - termed post-traumatic lobular metaplasia. Necrotizing sialometaplasia is generally unilateral, although midline and bilateral lesions have been reported.2
The lesion is self-limited and no treatment is usually necessary.
• Oropharynx : Squamous Cell Carcinoma
1 Svirsky, John. Necrotizing Sialometaplasia. eMedicine. Last updated on 10/28/08.
Available at: http://emedicine.medscape.com/article/1077574-overview
2 Thomspon LDR. Endocrine Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier; 2006: 283-286.
Carlson DL. Necrotizing sialometaplasia: a practical approach to the diagnosis.
Arch Pathol Lab Med. 2009 May;133(5):692-8.
Images courtesy of and copywrite by Dr. Jonathon McHugh, Dept. of Pathology, University of Michigan