
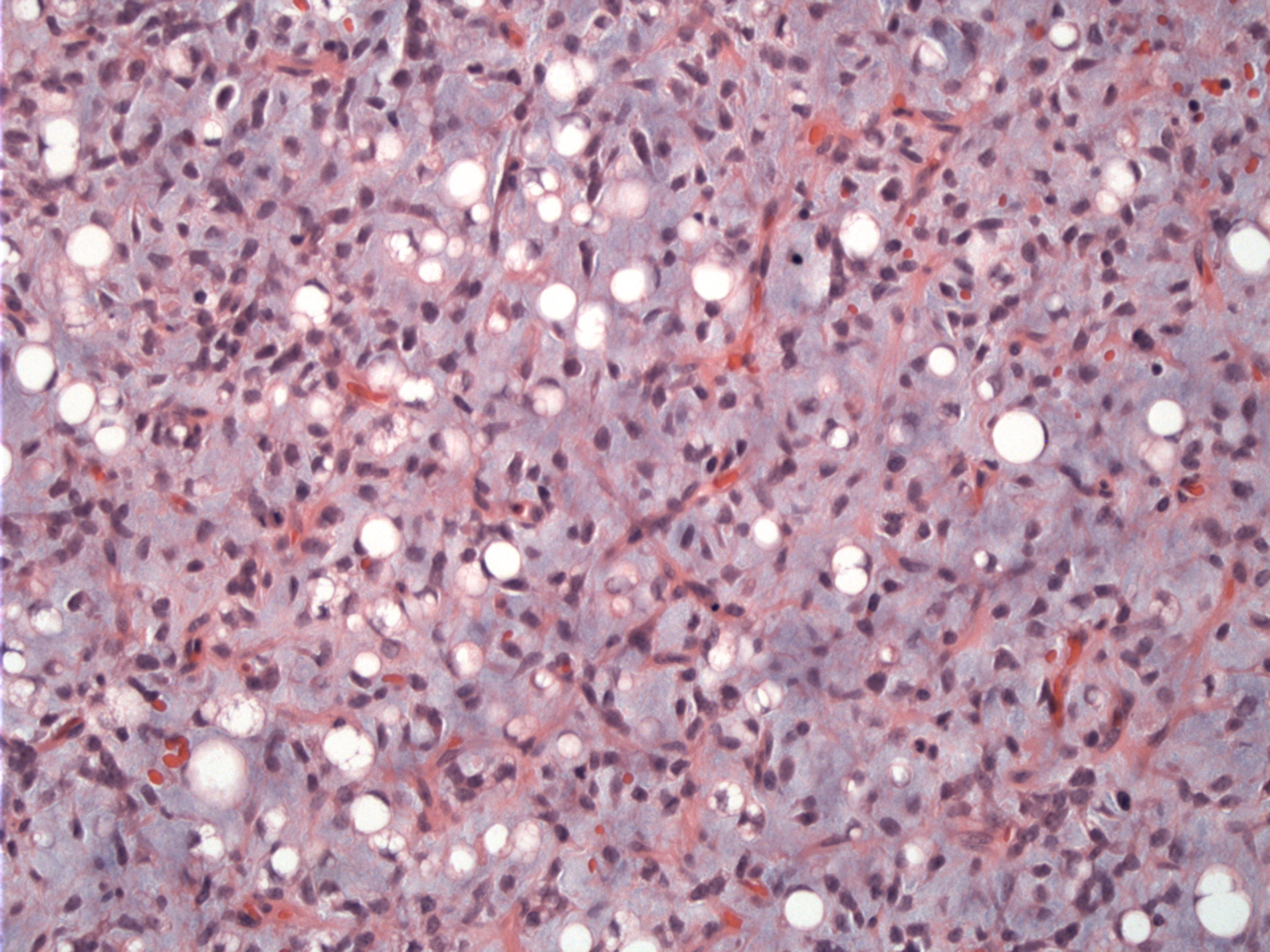
Case 1: This myxoid liposarcoma shows prominent branching pattern of capillaries throughout the tumor, in a so-called chicken-wire pattern.
Variably sized adipocytes are set in a myxoid background. Note the curvilinear vessels in a so-called chicken-wire or crows-feet pattern.
Lipoblasts are usually monovacuolated and cluster around vessels. Multivacuolated lipoblasts are most often located in the periphery of the tumor.
Diffuse CDK4 staining can be appreciated. Note that MDM2 and CDK2 stains are helpful in identifying liposarcomas. Staining for these markers is absent in deep lipomas and hence helps with their diagnostic separation (Aleixo; Binh).
Diffuse MDM2 positivity was also present.
p16 is quite strong as well and can be helpful in distinguishing liposarcomas from deep-seated lipomas (Mai).
Case 2: A pseudolymphangiomatous pattern or pseudoalveolar pattern due to mucin poolin and degeneration is highly suggestive of myxoid liposarcoma.
Lipoblasts can be appreciated here.
Another view of the pseudolymphangiomatous pattern with abundant mucin.
Liposarcomas are broadly divided into three main categories: well-differentiated, myxoid and pleomorphic. Myxoid liposarcomas account for one-third of liposarcomas and are characterized by a unique translocation t(12;16)(q13;p11) or less commonly t(12;22)(q13;q11-12). The DDIT3 gene on chromosome 12q13 fuses either to FUS on 16p11 or the EWS gene on 22q12 (Fletcher, Folpe).
Grossly, the tumor is gelatinous and firmer fleshier areas may indicate the presence of a round cell component. Histologically, small spindle cells and lipoblasts (usually univacuolated) are embedded in a myxoid matrix. There is a characterisitc background of delicate branching thin-walled capillaries, described as a chicken-wire or crow's feet pattern.
The high grade form of myxoid liposarcoma is round cell liposarcoma, which consists of hypercellular areas of undifferentiated round hyperchromatic cells. There is increased mitotic activity and nuclear overlap. The transition between the myxoid to round cell regions can be abrupt or gradual. The exact percentage required to diagnose a round cell liposarcoma is debated. The presence of any round cell component is probably worth mentioning in the report -- and greater than 25% connotes a high grade lesion (Folpe).
Liposarcomas typically occur in adulthood, with a peak incidence in the 5th through 7th decades. Parenthetically, liposarcomas are very rare in childhood and if present, occur between the ages of 10-15 and are of the myxoid subtype (Fletcher). Myxoid liposarcomas tend to arise in the limbs (versus the retroperitoneum in other variants).
→Myxoid liposarcomas exhibit a unique translocation involving the DDIT3 gene. The most common translocation is DDIT3-FUS t(12;16)(q13;p11) or less commonly DDIT3-EWS t(12;22)(q13;q11-12).
→Myxoid liposarcoma can transition to its high grade form, round cell liposarcoma.
• Lipomatous : Liposarcoma, Pleomorphic Type
• Lipomatous : Liposarcoma, Dedifferentiated Type
• Lipomatous : Liposarcoma, Myxoid and Round Cell Type
Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 1534-1539..
Folpe AL, Inwards CY. Bone and Soft Tissue Pathology: Foundations in Diagnostic Pathology Philadelphia, PA: Elsevier; 2010: 108-112.
Mai H, et al. P16 immunohistochemistry as an alternative marker to distinguish atypical lipomatous tumor from deep-seated lipoma. Applied Immunohistochemisty and Molecular Morphology 2009; 17: 51-56.
Aleixo PB, Hartmann AA, Menezes IC, Meurer RT, Oliveira AM. Can MDM2 and CDK4 make the diagnosis of well differentiated/dedifferentiated liposarcoma? An immunohistochemical study on 129 soft tissue tumours. J Clin Pathol. 2009 Dec;62(12):1127-35.
Binh MB, Sastre-Garau X, Guillou L, de Pinieux G, Terrier P, Lagacé R, Aurias A, Hostein I, Coindre JM.MDM2 and CDK4 immunostainings are useful adjuncts in diagnosing well-differentiated and dedifferentiated liposarcoma subtypes: a comparative analysis of 559 soft tissue neoplasms with genetic data. Am J Surg Pathol. 2005 Oct;29(10):1340-7.