
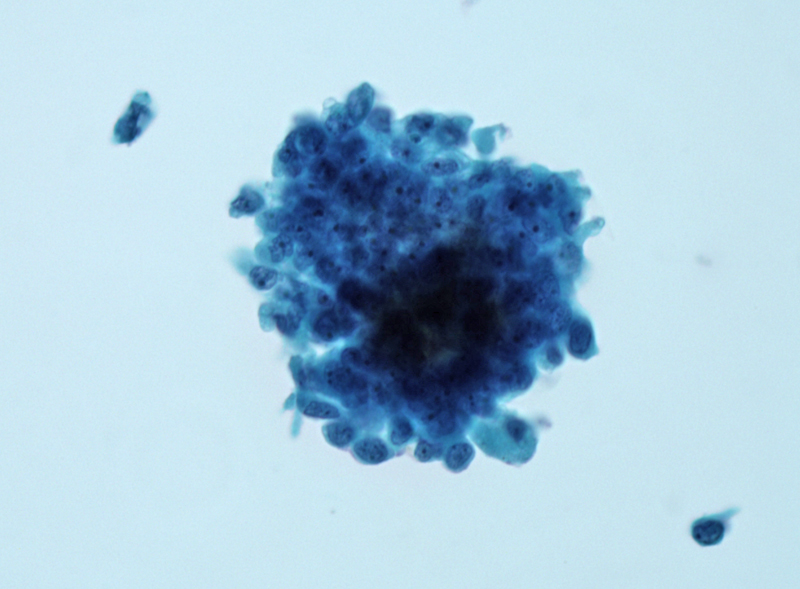
A monolayer prep shows a solid aggregate of follicular cells. The cells appear crowded and the architecture is irregular.
A very cellular region of the smear is seen. There is variation in size and shape, as well as nuclear crowding and overlap. A diagnosis of papillary carcinoma is not obvious.
A less cellular area shows the cytological features better, including large nuclei and micronucleoli.
Pre-op FNA demonstrates sheets of neoplastic cells.
The cells form a syncytium. The chromatin is cleared out and nucleoli are distinct.
Delicate fibrovascular septae separate solid islands of tumor cells.
The solid areas should comprise at least 50% of the tumor. The diagnosis of papillary carcinoma, again, is not obvious at this magnification.
The nuclear features are those seen in classic PTC, with cleared out chromatin, nuclear grooves, nuclear overlap and prominent small nucleoli.
At least six mitotic figures are seen in this field.
Punctate necrosis is focally seen here, but large areas of tumor necrosis are not characteristic of this variant.
A small focus with features of papillary architecture are present.
Here is a different case, which had mixture of tall cell and solid morphology. There was massive extrathyroidal extension in this instance.
The solid variant of papillary thyroid carcinoma (PTC) is comprised of at least 50% solid growth. The cells are arranged in sheets of cells intervened by fibrous stroma. There are vague papillary formations and the follicular pattern is partly maintained. The nuclear morphology is typical of papillary carcinoma.
BRAF mutations are prevalent and quite specific for PTC. Of interest, the particular type of BRAF mutation can help delineate the specific variant of PTC. For example, the BRAF V600E amino acid change is the most common mutation and is seen in classic, tall cell, oncoctyic and Warthin variants of PTC. The K601E mutation has only been seen in the follicular variant (Troncone).
Two recent case reports (Troncone, Trovisco) have identified a novel BRAF mutation leading to the replacement of a valine and lysine by glutamate i.e. BRAF (VK600-1E) or BRAF V600E + K601E. This mutation has only been in the solid variant and deserves further study.
This variant occurs more frequently in nuclear-accident associated PTC (Nikiforov).
Associated with aggressive behavior and high frequency of distant metastasis, in comparison with an age matched group of the classic variant of papillary thyroid cancers (Nikiforov). This variant should be distinguished from poorly differentiated (anaplastic) thyroid carcinoma, which has lower survival rates.
→More aggressive variant with poorer prognosis compared to classic PTC.
→Seen more frequently in nuclear-accident associated PTC.
→Novel BRAF mutation has been identified in a few cases of this uncommon variant.
• Thyroid : Papillary Thyroid Carcinoma, Cribriform-Morular Type
• Thyroid : Papillary Carcinoma, Tall Cell Variant
• Thyroid : Papillary Carcinoma, Oncocytic Variant
• Thyroid : Papillary Thyroid Carcinoma
• Thyroid : Papillary Carcinoma, Follicular Variant
Nikiforov YE, Erickson LA, Nikiforova MN, et al. Solid variant of papillary thyroid carcinoma: incidence, clinical-pathologic characteristics, molecular analysis, and biologic behavior. Am J Surg Pathol. 2001 Dec;25(12):1478-84.
Troncone G, Russo M, Malapelle U et al. Cytological and molecular diagnosis of solid variant of papillary thyroid carcinoma: a case report. Cytojournal. 2008 Mar 19;5:2.
Trovisco, Soares P, Soares R et al. A new BRAF gene mutation detected in a case of a solid variant of papillary thyroid carcinoma. Hum Pathol. 2005 Jun;36(6):694-7.
Author: Lina Aguirre MD, Endocrinology Fellow, University of New Mexico.