
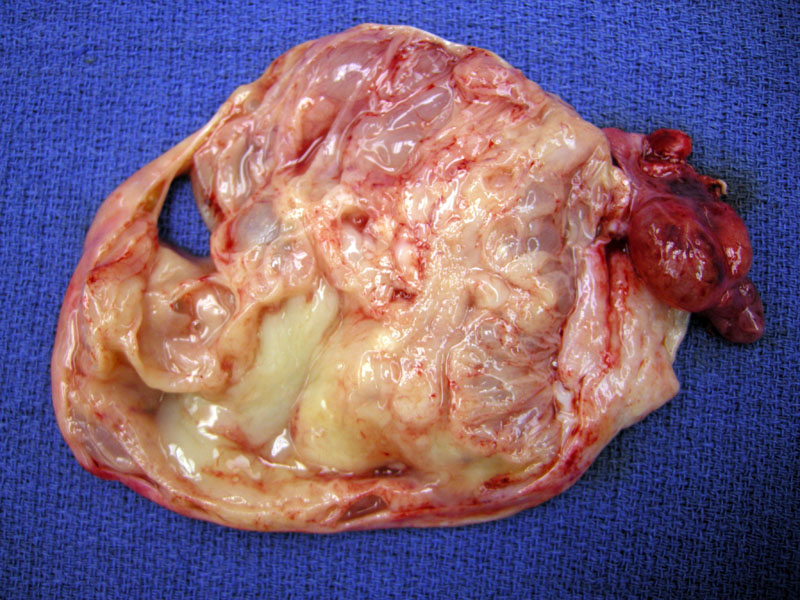
The tumor is composed of multiple variably sized cysts filled with mucoid and often tenacious cloudy fluid. A paratubal cyst and fimbria are seen at the right.
This intestinal-type borderline tumor demonstrates architectural complexity consisting of micropapillae in a filigree pattern. The lining cells are eosinophilic and contain mucin.
A banal orderly lining (lower image) abruptly transitions to an architecturally complex proliferation of atypical cells (upper image).
The proliferative epithelial cells are piled up and exhibit pseudostratification consistent with intestinal-type borderline mucinous tumor. Prominent cytologic atypia can be appreciated.
Variable cytological features within the same tumor can be appreciated, with areas of lower grade nuclei more akin to cystadenoma (right) compared to those with more prominent atypia (left).
Yet another area demonstrating pseudostratification and atypial nuclei. Note the lack of stromal invasion.
This different mucinous borderline tumor shows goblet cells scattered among the other epithelial cells in the lining.
Borderline mucinous tumors are almost as common as serous borderline tumors. They are classified into two subtypes: intestinal-type (85%) and endocervical (15%).
Intestinal-type mucinous borderline tumors (IMBT):
By far the most common type, the average age of diagnosis is between the late 40s to 50s. The vast majority of tumors are unilateral. The tumor is often larger than benign mucinous neoplasm and twice as large as endocervical-type borderline mucinous tumors. The cut surface is multiloculated.
Microscopic features include: (1) stratification of epithelial cells in no more than 3 layers; (2) mild to moderate cytologic atypia; (3) the lining is no longer flat like benign mucinous tumors, but is arranged in papillary folds which may be filiform (thread-like) and branching; (4) goblet cells, Paneth cells and neuroendocrine cells may be present.1,2
The diagnosis of "Mucinous borderline tumor with intraepithelial carcinoma" is ill-defined, but these tumors generally exhibit full-thickness atypia of the stratified epithelium.
Endocervical-type mucinous borderline tumors (EMBT):
Also known in the literature as "Mullerian Mucinous Papillary Cystadenoma of Borderline Malignancy and "Seromucinous Borderline Tumor", EMBT bears a remarkable histologic resemblance to serous borderline tumors. In fact, EMBT are often seen admixed with a component of serous borderline tumors, whereas IMBT are usually purely mucinous. Age at diagnosis ranges from 20 to 59 years (mean of 35), thus earlier than the intestinal-type variant. They are more often bilateral (40%) than the intestinal-type (5% bilateral). Furthermore, there is a strong association with endometriosis (up to 50% of cases).1,2
Grossly, they are smaller than intestinal-types (mean diameter of 8-10 cm versus >30cm in intestinal types). Similar to serous borderline tumors, papillary excrescences may be seen inside the cyst wall. Microscopic features include: (1) complex papillae with tufting similar to those seen in serous borderline tumors; (2) the lining cells are cuboidal or columnar with abundant eosinophilic cytoplasm and cilia; (3) goblet cells are absent; (4) a diffuse neutrophilic infiltrate is often seen in the stroma.
IHC studies may help differentiate between primary mucinous tumors of the ovary versus metastatic mucinous tumors from the GI tract. Endocervical-type mucinous borderline tumors are CK7+ and CK20- as expected of ovarian epithelial tumors.
However, distinguishing intestinal-type mucinous borderline tumors from metastatic mucinous GI tumors is a more complicated matter. Not surprisingly, intestinal-type mucinous borderline tumors exhibit intestinal differentiation. For example, they are CK7 positive, but may also be immunoreactive for CK20, CEA and CDX2 (IHC stains typically associated GI neoplasms). Although staining for the these three immunostains are often focal and less intense, sufficient overlap exists between IHC studies between primary ovarian mucinous tumors and those arising from the GI tract to make the diagnosis very difficult in certain situations.1,2
Treatment with unilateral salpingo-oophorectomy is sufficient if fertility is desired.
Over the long term, low malignant potential ovarian neoplasms often recur and require re-excision. Ultimately, patients suffer from repeated debulking surgeries with development of adhesions until complete resection is no longer possible. As many as 25% of patients will ultimately succumb to their disease.
♥ Mucinous borderline tumors are divided into intestinal types and endocervical types. By far, intestinal types predominate.
♥ Intestinal-types consist of papillary structures lined by pseudostratified mucinous cells. Goblet cells, Paneth cells and neuroendocrine cells (found in the intestine) are often seen as well.
♥ IHC can often distinguish between an endocervical-type mucinous borderline tumor from a metastatic colorectal cancer, but it is much harder to differentiated between an intestinal-type mucinous borderline tumor from a metastatic colorectal cancer.
• Ovary : Mucinous Cystadenocarcinoma (Infiltrative Type)
• Ovary : Mucinous Borderline Tumor, Endocervical Type
• Ovary : Mucinous Borderline Tumor, Endocervical-type (Case 2)
1 Nucci MR, Oliva Esther. Gynecologic Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier: 2009: 414-421.
2 Mills SE, ed. Sternberg's Diagnostic Surgical Pathology.4th Ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004: 2554-2556.
3 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 576-7.
Ronnett BM, Kajdacsy-Balla A, Gilks CB et al. Mucinous borderline ovarian tumors: points of general agreement and persistent controversies regarding nomenclature, diagnostic criteria, and behavior. Hum Pathol. 2004 Aug;35(8):949-60.
Hart WR. Mucinous tumors of the ovary: a review. Int J Gynecol Pathol. 2005 Jan;24(1):4-25.