
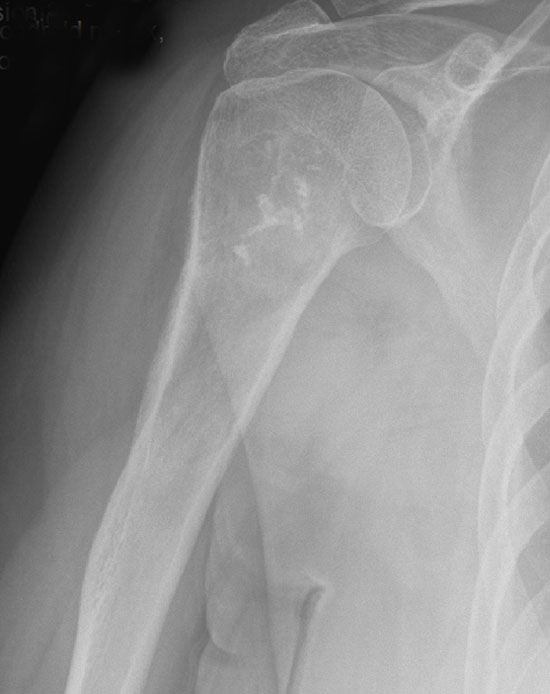
There is a lytic proximal humeral bone lesion with a thickened cortex, matrix production, endosteal erosion and irregular calcifications. This picture is very typical for chondrosarcoma.
This FNA demonstrates nuclear enlargement, hyperchromasia and pleomorphism. In Grade 2 chondrosarcomas, the chrondocyte nuclei should be approximately 2x larger than nuclei of non-neoplastic chondrocytes.
Neoplastic chondrocytes show coarse chromatin with multiple nucleoli and irregular nuclear contours, although the last feature is not obvious in this image. The background shows a loose myxoid quality.
Single malignant chondrocytes are present within a myxo-chondroid background. The cells are round to oval, and one can easily imagine them as chondroid in nature.
A corresponding FNA Diff-Quik images demonstrates high cellularity and chondrocytes with enlarged nuclei. Binucleate chondrocytes are present. The cells are embedded in a metachromatic chondroid matrix
This grade 1 chondrosarcoma shows only a very minimal increase in cellularity and certainly could pass in this image as an enchondroma.
This tumor is slightly more cellular and contains an occasional binucleated cell (arrow).
This image demonstrates an intermediate grade conventional chondrosarcoma with increased cellularity, moderately enlarged and atypical chondrocytes. The matrix produced by the neoplastic chondrocytes can be either hyaline, myxoid or both in varying proportions. You know its not a grade 1 when it is easy to tell this from an enchondroma.
This grade 3 chondrosarcoma retains its lobular architecture only vaguely.
The grade 3 chondrosarcoma is much more cellular and atypia is widespread. Nuclei are dark and crowded.
Mitotic figures (arrows) are easily found. High grade tumors also have necrosis frequently.
Chondrosarcoma, a malignant tumor of hyaline cartilege, accounts for 15% of all malignant bone tumors (Folpe) and is the 3rd most common malignant bone tumor after osteosarcoma and myeloma (Fletcher). Conventional chondosarcomas have a predilection for the shoulder and pelvic girdles and very very rarely involve the small bones of hands and feet.
There are several ways to categorize chondrosarcomas: by location (e.g. periosteal, parosteal, chondrosarcoma of small bones), by histology (e.g. conventional, clear cell, dedifferentiated, mesenchymal) or by clinical features (e.g. primary versus secondary). Secondary chondrosarcoma arise from pre-existing lesion such as an osteochondroma. Periosteal chondrosarcoma occur on the surface of the bone versus the more common intramedullary location. Clear cell, dedifferentiated and mesenchymal chondrosarcoma are other rare variants with unique clinicopathologic features that will be discussed in separate cases.
As for most bone tumors, radiology is extremely helpful and in some cases, diagnostic. The classic radiographic image for chondrosarcoma is that of expanded bone with an overlying thickened cortex. Scattered calcifications may be seen in the radiolucent lesion. Conventional chondrosarcomas arise in the medullary bone and eventually, break through the cortex to form a soft tissue mass.
Grossly, the lesion would contain pearly white-blue areas because that is the color of the cartilaginous component. The microscopic appearance varies depending on the grade of the tumor and in low-grade lesions, it may be difficult to distinguish from a benign enchondroma. The permeation and entrapment of trabeculae can be a helpful finding (Folpe, Fletcher).
The grading for chondrosarcomas does not rely on mitotic figures, rather, it is determined by degree of cellularity and nuclear changes of the chondrocytes.
- Grade 1: Very difficult to differentiated from benign enchondromas, but these lesions should show increased cellularity with enlarged, irregular chondrocytes.
- Grade 2: Increased cellularity compared to Grade 1 with even more prominent nuclear enlargement and atypia. Binucleate cells can be seen.
- Grade 3: Pronounced cellularity with pleomorphic hyperchromic chondrocytes. Binucleate cells are common. Spindling of cells occur at the periphery of the tumor.
Note that chondrosarcoma of hands and feet is extremely rare. Enchondromas of small bones can exhibit hypercellularity and nuclear enlargement, features that would elicit concern in the larger bones. Therefore, to diagnose chondrosarcoma of the small bones, there must be radiographic evidence of cortex transgression or soft tissue involvement (Folpe).
Affects patients in 4th through 6th decade of life. Presents as a painful enlarging mass, most commonly the pelvis followed by the shoulder girdles and ribs (i.e. axial skeleton).
These tumors are generally indolent; recurrence and metastasis can occur up to 20 years after initial diagnosis. Risk of metastasis and prognosis correlates with histologic grade. For example, risk of distant metastasis for grade 1 tumors is 4% and up to 30% for higher grade tumors. Overall five year survival is approximately 77% (Fletcher).
→Chondrosarcomas are the third most common malignant tumor of bone.
→Histologic grade has prognostic significance and is determined by cellularity and nuclear pleomorphism. Mitotic activity is not used.
→Radiologic features can be diagnostic if expansion of bone, thickened cortex and irregular calcifications within the mass.
→It is difficult to differentiated grade I chondrosarcoma from enchondroma.
→Chondrosarcoma is quite rare in the small bones of hands and feet, so think enchondroma unless there is compelling evidence to the contrary.
• Chondroid : Chondrosarcoma, Myxoid Type
Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007:1608-1610.
Folpe AL, Inwards CY. Bone and Soft Tissue Pathology: Foundations in Diagnostic Pathology Philadelphia, PA: Elsevier; 2010: 324-5.
Silverberg SG. Silverberg's Principles and Practice of Surgical Pathology and Cytopathology. Philadelphia, PA: Elsevier; 2006:715-8.