
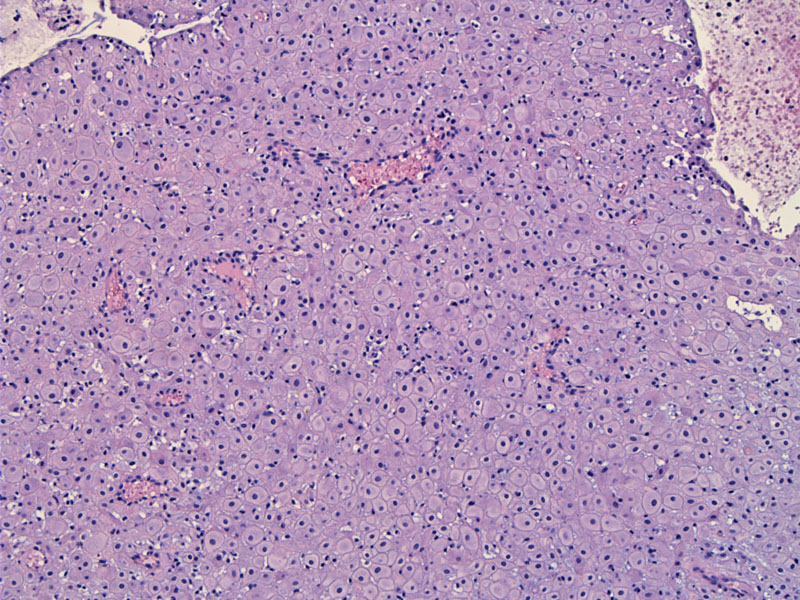
Some fragments show confluent areas of stromal decidualization indication of progestin effect.
However, while progestin effect in the form of decidualization is seen (upper right), there is also a fragment of endometrium showing complexity. The gland-to-stroma ratio is high and the glands have a complex contour.
Yet another fragment showing the same changes, consistent with residual hyperplasia in a background of partial response. The area to the left shows confluent stromal decidualization consistent with progestin effect.
High-dose progestin therapy is frequently used to treat endometrial hyperplasia, complex atypical hyperplasia (CAH) and well-differentiated adenocarcinoma (WDC). This is a good option for women who are poor surgical candidates and for women who wish to preserve their fertility. High-dose progestin (Provera, Megace or Depo-Provera) are given and a biopsy is usually taken between 2-6 months to evaluate treatment response.
Histologically, one typically sees stromal decidualization. Depending on the pre-treatment diagnosis, the glandular architecture may vary. For example, complete resolution would result in benign appearing glands (proliferative, secretory or atrophic). In regression or partial response, the glands would appear as hyperplastic without atypia (if initial biopsy was CAH or WDC). Some cases of CAH or WDC are not responsive to progestin therapy and will persist and/or progress to higher grade lesions.
Wheeler (2007) studied 44 patients with CAH or WDC treated with progestin and demonstrated that the majority of cases showed a robust response. Decreased gland-to-stroma ratio, decreased glandular cellularity, decreased to absent mitotic activity and loss of cytologic atypia were seen in post-treatment biopsies obtained 3-6 months after progestin therapy was initiated.
Twelve (67%) of 18 women with CAH had complete resolution, 2 (11%) regressed to complex hyperplasia without atypia, and 4 (22%) demonstrated persistent disease. Eleven (42%) of 26 women with WDC had complete resolution and 15 (58%) had persistent disease. The follow-up period was approximately 12 months. The authors also found that if cytologic atypia persists at 6 months, the lesion is unlikely to respond to therapy and a hysterectomy would be recommended.2
Reed (2009) also found similar results in a study of 70 women with atypical hyperplasia. 26.9% of those treated with progestin and 66.7% of those not treated had persistence/progression. Thus, progestin treatment was associated with a lower likelihood of persistence/progression. Note, however, that there is always a subset of women (25% in this study) who do not respond to progestin therapy.3
• Endometrium : Simple Hyperplasia Without Atypia
1 Robboy SJ, Anderson MC, Russell P. Pathology of the Female Reproductive Tract. London, UK: Churchill Livingstone; 2002: 279-281.
2 Wheeler DT, Bristow RE, Kurman RJ. Histologic alterations in endometrial hyperplasia and well-differentiated carcinoma treated with progestins. Am J Surg Pathol. 2007 Jul;31(7):988-98.
3 Reed SD, Voigt LF, Newton KM et al. Progestin therapy of complex endometrial hyperplasia with and without atypia. Obstet Gynecol. 2009 Mar;113(3):655-62.