
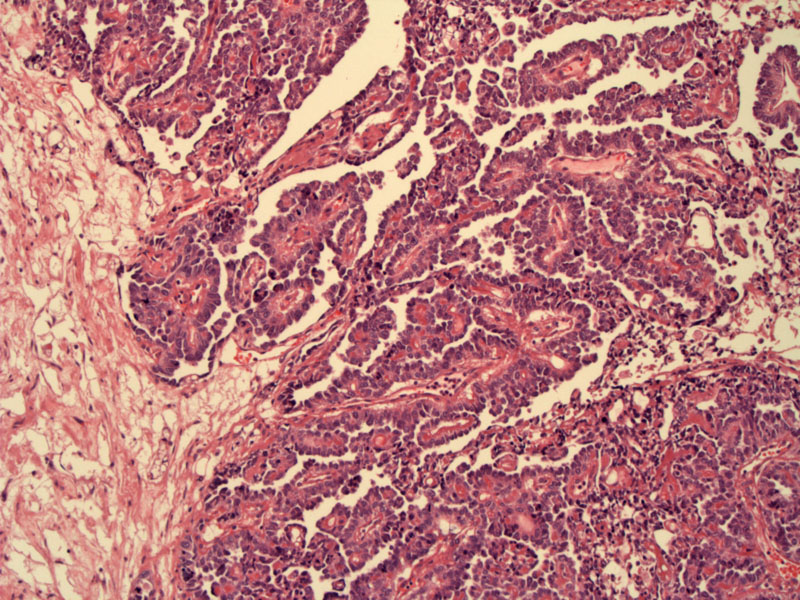
An endodermal sinus pattern (aka pseudopapillary or festoon pattern) is seen here. There is a proliferation of papillary structures and anastamosing glands.
The papillary structures are lined by neoplastic cells with amphophilic cytoplasm (and sometimes clear) and atypical hyperchromatic nuclei with prominent nucleoli.
The most distinctive feature histological feature of this pattern are Schiller-Duval bodies. It is papillary structure containing a central blood vessel surrounded by a rim of loose mesenchyme with an outer mantle of cuboidal or columnar neoplastic cells. The whole structure projects into a cystic space lined by attentuated neoplastic cells.
There are often a mixture of patterns. Here, the papillary structures (lower left) merge with the reticular/microcystic pattern (upper and right). A delicate network of anastamosing glands and cystic structures are lined by neoplastic cells. Note the presence of intracellular and extracellular hyaline globules, which are characteristic but not pathognomonic of YST.
Yolk sac tumors (YST), formerly known as endodermal sinus tumor, are the second most common germ cell tumor among young females. Pure YST is very rare in peri or postmenopausal women, but YST may arise in association with surface epithelial ovarian neoplasms in this older age group.
Microscopically, a myriad of patterns is seen as the tumor attempts to recapitulate yolk sac structures. The most common is a reticular pattern composed of a network of channels and spaces lined by the lesional cells; this pattern frequently merges with the microcystic pattern.
The most distinctive pattern is the festoon or pseudopapillary pattern which exhibit the trademark Schiller-Duval bodies, although these are only found in 30% of cases. Other patterns include parietal (characterized by thickened basement membrane), polyvesicular (multiple pear-shaped cystic structures resembling primitive gut), hepatoid and glandular differentiation.1
YST are PAS positive as the tumor cells contain glycogen; the tumor is also AFP-positive.
Mean age of diagnosis is 19. Typically presents with a rapidly enlarging abdomen and rarely, endocrinologic manifestations such as virilization. High levels of serum AFP are detected and some patients have elevated CA-125 as well.
Clinically, the tumor is almost always unilateral and large (median diameter of 15 cm). The external surface is smooth and the cut surface is grey-tan and fleshy. Cysts and secondary degenerative changes such as hemorrhage and necrosis are common.
Two-thirds of patients present at stage I and the remainder have advanced disease. YST tends to spread similarly to surface epithelial ovarian tumors (peritoneum, omentum, liver, pelvic lymph nodes). AFP is a good marker to measure treatment response and tumor recurrence.
Unilateral salpingo-oopherectomy and staging are considered adequate for stage I tumors. Cytoreductive surgery and chemotherapy are added for more advanced disease. Because of this tumor's sensitivity to chemotherapy, some clinicians employ chemotherapy for stage I tumors to achieve an even better response. Multiple combination chemotherapy regimens have been employed successfully.
Stage is the most important prognostic factor. With the advent of combination chemotherapy, there is overall survival rate of 80% for stage I tumors and 50% for advanced disease.2
♥ Schiller-Duval bodies, although seen in only 30% of YST, are highly characteristic of YST.
♥ There is a remarkable range of histologic patterns as this tumor attempts to recapitulate structures seen in the yolk sac. Some common patterns include microcystic, reticular, pseudopapillary or festoon, parietal, hepatoid and glandular.
♥ AFP is a good marker to measure treatment response and tumor recurrence.
♥ YST is a tumor of young women with mean age of 19 at diagnosis.
• Mediastinum : Yolk Sac Tumor
• Testis : Pure Yolk Sac Tumor
1 Nucci MR, Oliva Esther. Gynecologic Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier: 2009: 513-520.
2 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 284-6.