
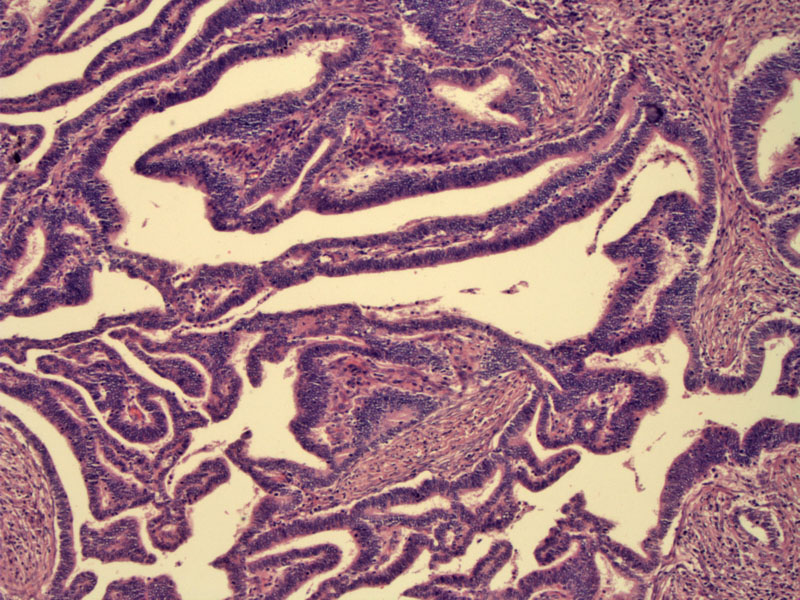
Papillae are lined with well-differentiated glandular cells. The stroma is fibrous with scattered inflammatory cells.
The glandular cells lining the papillary structures resemble endocervical or occasionally, endometrial cells. They are pseudostratified and with mild cytologic atypia. If moderate cytologic atypia is seen, the diagnosis must be questioned.
Villoglandular adenocarcinoma (VGA) is a rare variant of cervical adenocarcinoma. The WHO defines villoglandular papillary adenocarcinomas as "tumors with a villoglandular pattern and epithelial cells that are generally moderately to well differentiated". VGA typically has a pushing border and is associated with high-risk HPV subtypes 16 and 18.1,2
Microscopically, there is proliferation of slender papillary structures lined by a pseudostratified columnar cells exhibiting mild cytologic atypia. The stroma is fibrous and contains scattered inflammatory cells. The tumor tends to invade with a pushing border of broad tubules and nests rather than single infiltrative glands.3 A clear demarcation between the broad tumor base and underlying cervical stroma is usually present.1
The pathologist must exercise extreme caution in diagnosing this tumor because a well-differentiated villoglandular tumor is equated with an indolent, almost benign entity in the mind of many clinicians. In fact, some clinicians may even perform a local excision (cone biopsy) instead of a more involved surgery. It is important to note that conventional adenocarcinomas may contain villoglandular components. Alternatively, a villoglandular adenocarcinoma may have adjacent conventional adenocarcinoma (in situ or invasive). Therefore, a true villoglandular adenocarcinoma must demonstrate both mild cytologic atypia and a lack of co-existing conventional adenocarcinoma elements.
Numerous reports exist where the diagnosis of villoglandular adenocarcinoma was made resulting in conservative treatment. These patients subsequently developed recurrent and metastatic tumors, most likely due to missed components of invasive conventional adenocarcinomas present in the original tumor.4,5 Unfortunately, a concise definition of this entity has not been established and the diagnostic criteria are murky in all the authoritative texts. Thus, a comprehensive review of villoglandular lesions in the cervix is well overdue.
VGA is typically a well-differentiated tumor that occurs in women in their 40s and presents with abnormal vaginal bleeding. Grossly, the tumor forms an exophytic friable papillary mass.2
While a small biopsy specimen can indicate that growth is of villoglandular pattern, conization is required to determine if the tumor is purely a villoglandular type. Once diagnosed, treatment can proceed according to stage by the same guidelines as cervical adenocarcinoma.
Prognosis is favorable if one applies the diagnostic criteria with rigor. There should be only mild cytologic atypia and no other types of adenocarcinomas are present within the tumor.
♥ The diagnosis of well-differentiated villoglandular adenocarcinoma must be made with caution as clinicians often associate this entity with an indolent benign course and exercise conversative treatment.
♥ Usually has a broad pushing border.
♥ Associated with high-risk HPV types 16 and 18.
• Cervix : Adenocarcinoma in situ
• Endometrium : Endometrioid adenocarcinoma, Villoglandular Variant
1 Nucci MR, Oliva Esther. Gynecologic Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier: 2009: 180-1.
2 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 706-7.
3 Sternberg SS, ed. Diagnostic Surgical Pathology.4th Ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004: 2416-7.
4 Macdonald RD, Kirwan J, Hayat K et al. Villoglandular adenocarcinoma of the cervix: clarity is needed on the histological definition for this difficult diagnosis. Gynecol Oncol. 2006 Jan;100(1):192-4.
5 Heatley MK. Villoglandular adenocarcinoma of the uterine cervix-a systematic review of the literature. Histopathology. 2007 Aug;51(2):268-9.