
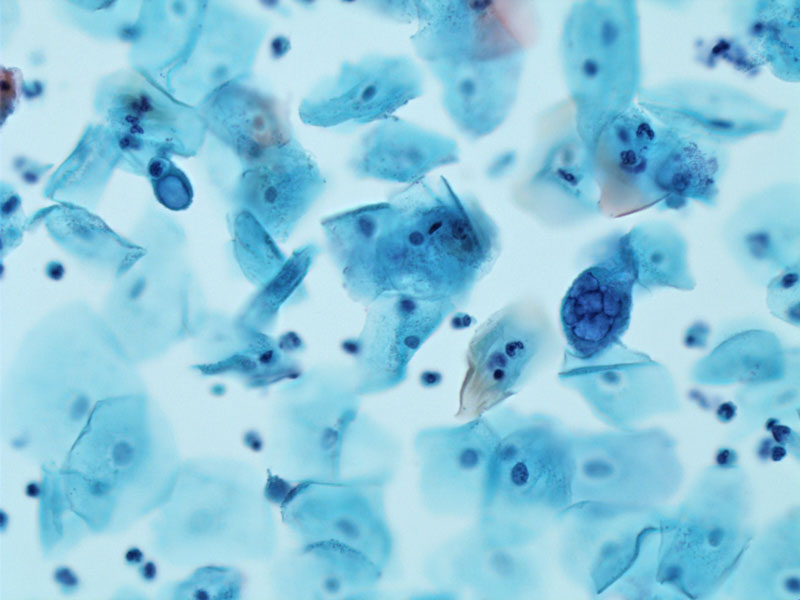
Two infected cells are seen in this cytology preparation. One that is multinucleated (center right) and the other (upper left) with a 'ground-glass' chromatin pattern.
Intranuclear inclusions push the host chromatin to the periphery, thus, accentuating the nuclear rim.
An enlarged multinucleated cell is seen at the top, left of center.
Cowdry type A inclusions which contain virions push the host chromatin to the periphery. The dark bodies surrounded by a clear halo are the inclusion bodies.
This enlarged multinucleated cell contains glassy peripherally marginated chromatin. Nuclear overlap and molding is also seen.
Sometimes necrotic epithelial cells are seen in pap smears with HSV infection.
Another area showing necrotic squamous cells clustered in the middle of this image.
In contrast to their easy recognition via cytology, affected cells can be more difficult to detect in the ulcerated areas by histology. Degenerative atypia seen in early cell death can overlap with viropathic changes. The abrupt ulceration is a strong clue.
In such cases, IHC for herpes virus antigen is highly useful. Strong nuclear reactivity is seen in the affected area.
Herpes infection in the female genital tract is usually due to HSV-2 and much less frequently, HSV-1. Microscopically, the infected squamous cells demonstrate the following viropathic changes: (1) multinucleation (2) nuclear molding (3) ground-glass chromatin that is peripherally marginated and (4) Cowdry type A intranuclear inclusion bodies. Diagnosis is based on scraping the base or edge of an ulcer and finding the hallmark cytologic features on a cytology (Tzanck) preparation. IHC stains for herpesvirus antigens can also be helpful.
The prodrome includes pain or burning in the affect area. Some patients may experience systemic symptoms such as fever, headache and lymphadenopathy. Vesicles and ulcers soon appear and can involve the squamous epithelium of the vulva, vagina, cervix, bladder, urethra and anus. Rarely, it may ascend to involve the endometrium. Primary infections can be very painful and may last 2-6 weeks. Subsequent episodes are usually milder with fewer lesions.
Transmission of HSV-2 to the neonate during passage through an infected birth canal can cause fulminant neonatal disease including lymphadenopathy, splenomegaly and necrotic foci in the viscera (lungs, liver, adrenals) and CNS.2 This systemic infection more frequently results from vaginal delivery during a primary outbreak rather than a recurrence.
Antiviral medications such as acyclovir are mainstays of treatment of symptomatic outbreaks. In addition suppressive therapy with these medications results in fewer recurrences and decreased transmission rates.
Women with a prodrome or active lesions often undergo cesarean delivery in order to prevent neonatal transmission.
Once acquired, it is impossible to completely eradicate this infection. Patients will experience variable frequencies of recurrence. Patients who are immunosuppressed tend to experience more frequent and more severe outbreaks.
→Cytologic features of herpes infection include: multinucleation, nuclear molding, chromatin margination, ground-glass nuclei and Cowdry type A intranuclear inclusions.
1 Nucci MR, Oliva Esther. Gynecologic Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier: 2009: 83-4.
2 Kumar V, Abbas AK, Fausto N. Robbins and Cotran Pathologic Basis of Disease. 7th Ed. Philadelphia, PA: Elsevier; 2005: 365-6.