
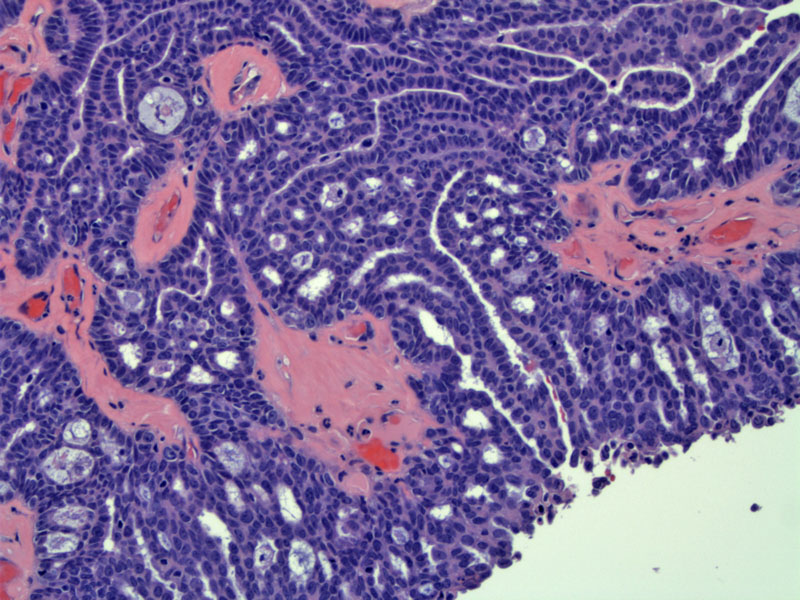
Micropapillary architecture is demonstrated by marked epithelial proliferation consisting of multiple slender papillae.
Note that the papillae arise directly from the stromal cores in contrast to hierarchical branching seen in conventional serous tumors.
A closer look reveals small filiform papillae with cores containing little or no stroma emanating from large edematous or myxoid stalks.
Kurman and colleagues at John Hopkins University have proposed that we abandon the term "borderline serous tumors" or "serous tumors of low malignant potential, SLMP" altogether. Instead, we ought to categorize these tumors as either "atypical proliferative serous tumor" and "micropapillary serous carcinomas". The rationale behind this reclassification is that a serous tumors with a micropapillary pattern show a higher frequency of invasive implants and tumor progression and ought to be called "carcinomas", whereas the majority of borderline tumors are indolent and rarely progress and ought to be renamed with the more benign term "atypical proliferative serous tumor" (Kurman). Supporting this new classification scheme is the recent discovery that the gene expression profile of LMP-MP is similar to low grade serous carcinoma and distinct from the usual type LMP, a profile which may explain in part their more aggressive clinical behavior (May).
However, there are pathologists who do not agree with this proposed Kurman scheme. A recent study by Deavers and colleagues at MD Anderson compared 18 cases of micropapillary or cribriform
pattern (MP/CP) against 81 cases of typical borderline serous tumors (SLMP). They found that 17% of MP/CP cases had invasive implants versus 6% in SLMP cases and 78% of MP/CP patients had recurrence or progression of disease versus 31% in SLMP patients.
The authors concluded that MP/CP tumors were more likely to: (1) have bilateral ovarian involvement; (2) exhibit invasive implants; (3) have more frequent recurrence with shorter progression-free interval. Thus, these features support Kurman's assertion that micropapillary serous tumors are different tumors than the usual SLMP. However, the overall survival of MP/CP patients did not significantly differ from usual SLMP patients, and furthermore, when usual SLMP patients are followed over an extended period of time, a number of patients will do progress into carcinomas -- thus, this group believes that micropapillary serous tumors still belong in the SLMP family (Deavers).
Data suggests that having the micropapillary pattern alone does not imply an unfavorable prognosis; only such tumors with invasive implants seem to behave aggressively (Prat, Eichhorn). At least four investigations have failed to demonstrate that the overall survival of patients with advanced stage SBTs-MP differs from patients with typical SBTs (Eichhorn; Prat; Slomovitz; Deavers). They have shown that bilaterality, ovarian surface growth, and advanced stage are more common in SBTs-MP than of typical SBTs, but a strong association of the former tumors with invasive implants and poor outcome has not been confirmed.
♣ Micropapillary architecture is one of the constellation of histologic features that warrant mentioning on the pathology report. It is associated with tumor progression, bilateral ovarian involvement and invasive implants. Note, however, micropapillary architecture has not been shown to be an independent prognostic factor.
• Ovary : Serous Borderline Tumor
• Ovary : Serous Cystadenofibroma
• Ovary : Serous Borderline Tumor
• Ovary : Serous Borderline Tumor with Invasive Implants
• Ovary : Serous Borderline Tumor with Non-invasive Implants
• Ovary : Serous Carcinoma, Low Grade
• Ovary : Serous Adenocarcinoma, High Grade Papillary
Deavers MT, Gershenson DM, Tortolero-Luna G, et al. Micropapillary and cribriform patterns in ovarian serous tumors of low malignant potential. A study of 99 advanced stage cases. Am J Surg Pathol 2002; 26:1129–41.
Eichhorn JH, Bell DA, Young RH, Scully RE. Ovarian serous borderline tumors with micropapillary and cribriform patterns: a study of 40 cases and comparison with 44 cases without these patterns.Am J Surg Pathol. 1999 Apr;23(4):397-409.
Kurman RJ, Seidman JD, Shih I-M. Serous borderline tumors of the ovary. Histolopathology 2005;47:310-8.
May T, et al. Low malignant potential tumors with micropapillary features are molecularly similar to low-grade serous carcinoma of the ovary. Gynecol Oncol. 2010 Jan 29.
Prat J, De Nictolis M. Serous borderline tumors of the ovary: a long-term follow-up study of 137 cases, including 18 with a micropapillary pattern and 20 with microinvasion. Am J Surg Pathol. 2002 Sep;26(9):1111-28.
Slomovitz BM, Caputo TA, Gretz III, HF et al. A comparative analysis of 57 serous borderline tumors with and without a noninvasive micropapillary component. Am J Surg Pathol 2002; 26:592–600.
Yemelyanova A, Mao TL, Nakayama N, Shih IeM, Kurman RJ. Low-grade serous carcinoma of the ovary displaying a macropapillary pattern of invasion. Am J Surg Pathol. 2008 Dec;32(12):1800-6.