
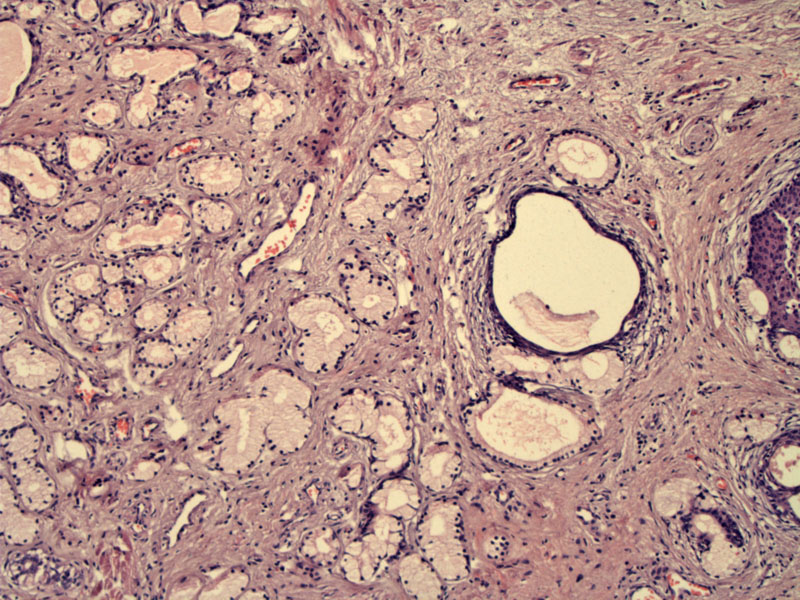
Normal Bartholin gland acini are seen here lined by columnar mucinous cells. It may look like an abnormal proliferation at first glance, but is truly benign. A dilated duct is seen just off center.
The dilated cyst is usually lined by a simple columnar-type epithelium. The lining cells may occasionally be ciliated or squamous cells.
Bartholin glands are paired glands located at approximately the 4 and 8 o'clock positions of the labia minora. Their function is to secrete mucus and moisten the vestibule. Normally, they are non-palpable. However, the ducts can become blocked, forming cysts and abscesses. Very rarely, adenocarcinoma of the Bartholin gland can occur.
Histologically, Bartholin's glands are composed of: (1) a cluster of acini lined by mucus-secreting columnar cells and (2) a duct lined by transitional epithelium. The mucinous secretions are carried by the duct, which terminates at the vestibule of the vagina. Bartholin gland cyst arises from dilation of the duct.
The cyst wall may contain inflammatory cells and either normal or atrophic acini. Occasionally, the inflammation may be so vigorous as to obscure the cyst lining. However, identification of residual mucinous glands embedded in a fibrotic and inflammed stroma will be helpful.
Most common in females in the 20s. If not infected, a painless lump is felt. Infected cysts are typically very painful.
The treatment depends on several factors related to the cyst: the cyst size , how painful it is, and if there is secondary infection. Often small cyst can be treated by soaking in warm water (sitz bath) several times a day for 3 or 4 days to allow it to rupture and drain. Incision and drainage is usually the first line therapy of abscesses. Recurrent cysts or abscesses may be marsupialized, ablated, or excised.
Occasionally, the cysts may recur. Abscesses may form in the duct from bacterial infections (especially gonorrhea).1 Very rarely, a carcinoma (squamous cell carcinoma, adenocarcinoma or transitional cell carcinoma) may arise from the epithelial lining of the duct.
1 Rosai, J. Rosai and Ackerman's Surgical Pathology. 9th Ed. Philadelphia, PA: Elsevier; 2004: 1498.
2 Mills SE, ed. Sternberg's Diagnostic Surgical Pathology.4th Ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004: 2335.
3 Mills, S. Histology for Pathologists. 3rd Ed. Philadelphia, PA: Lippincott, Williams & Wilkins; 2007: 985-6.
**Images courtesy of Dr. Lida Crooks, VAMC Albuquerque NM.