
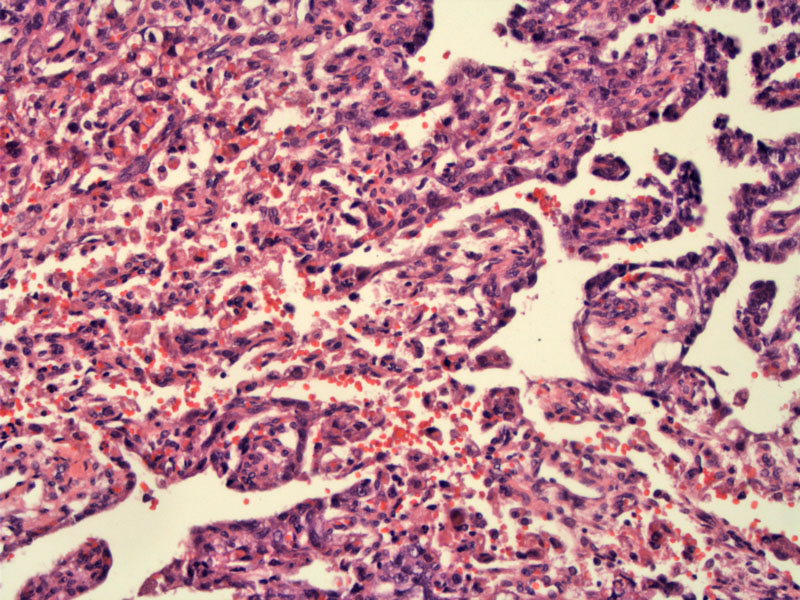
This vaginal YST arose in a 1 yo girl and demonstrates mixed patterns (endodermal and reticular/solid patterns).
A remnant of vaginal squamous mucosa (center) is surrounded by tumor consisting of edematous stroma and cystic glands.
There are areas of sclerosis which also represent invasion into vulvar stroma.
Here is an area of malignant clear cells that may be confused with clear cell carcinoma.
Another region of the tumor exhibits papillary structures. No clearly identifiable Schiller-Duval bodies were seen.
Surface epithelium of the vagina (left image) overlies tumor with microglandular structures and edematous stroma.
Malignant germ cell tumors account for only 3% of pediatric malignancies. The most common subtype is yolk sac tumor (formerly called endodermal sinus tumor). Yolk sac tumors (YST) are most frequently located in the sacrococcygeal region, gonads and mediastinum. The vagina is an infrequent site (Watanabe) and only 50 vaginal YSTs have been documented in the literature thus far (Kumar).
Vaginal YST may be mistaken clinically as botryoid rhabdomyosarcoma as it can present as a polypoid mass protruding from the vagina. Histologically, the presence of optically clear pleomorphic cells may lead to misdiagnosis as clear cell adenocarcinoma (Gangopadhyay).
Several key histologic features can help you identify YST: (1) presence of Schiller-Duval bodies; (2) PAS-positive eosinophilic hyaline globules; (3) IHC positive staining for AFP.
Vaginal bleeding is the typical presentation; a protruding mass and difficulty with urination have also been reported (Arora).
Occurs exclusively in young girls less than 3 yrs of age. Serum AFP level is a useful marker for diagnosis and monitoring recurrence.
Resection with combination chemotherapy is recommended.
This is a locally aggressive tumor capable of metastasis. Untreated patients have died within 2 to 4 months of presentation (Anderson). Conservative surgery is advised to maintain sexual and reproductive function, but actually radical surgery may be necessary depending on the infiltration of the tumor to the surrounding structures.
• Mediastinum : Yolk Sac Tumor
• Testis : Pure Yolk Sac Tumor
Anderson WA, Sabio H, Durso N. Endodermal sinus tumor of the vagina: the role of primary chemotherapy. Cancer 1985; 56: 1025–1027.
Arora M, Shrivastav RK, Jaiprakash MP. A rare germ-cell tumor site: vaginal endodermal sinus tumor.Pediatr Surg Int. 2002 Sep;18(5-6):521-3.
Gangopadhyay M, Raha K, Sinha SK et al. Endodermal sinus tumor of the vagina in children: a report of two cases. Indian J Pathol Microbiol. 2009 Jul-Sep;52(3):403-4.
Kumar V, Kini P, Vepakomma D et al. Vaginal endodermal sinus tumor. Indian J Pediatr. 2005 Sep;72(9):797-8.
Watanabe N, Okita H, Matsuoka K et al. Vaginal yolk sac (endodermal sinus) tumors in infancy presenting persistent vaginal bleeding. J Obstet Gynaecol Res. 2010 Feb;36(1):213-6.
****Images courtesy of Dr. Lida Crooks, VAMC Albuquerque New Mexico.