
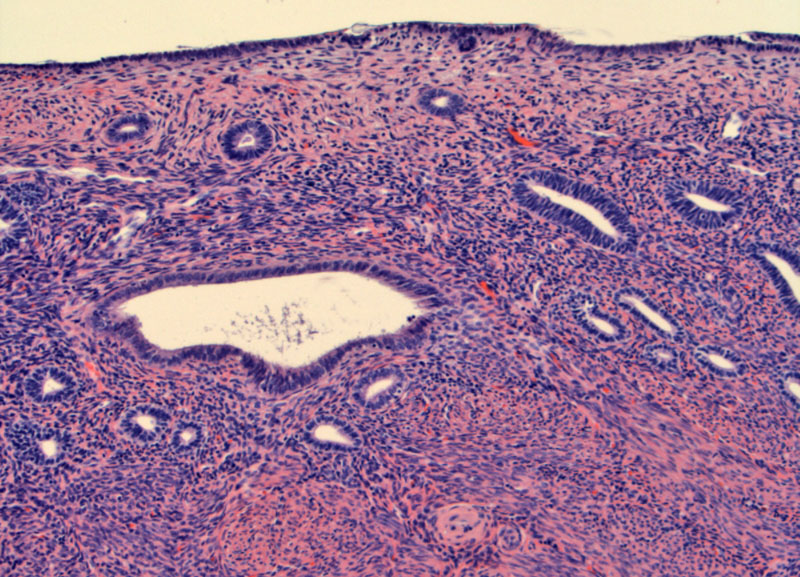
Atrophic endometrium shows an attenuated thickness, with occasionally enlarged glands and otherwise simple small tubular glands.
Another hysterectomy shows cystic atrophy with scant simple tubular glands lined by cuboidal epithelium. Some pink material is seen within the lumens.
Endometrial biopsy most often will yield only scant material consisting of blood and detached strips of simple glands.
Fragments of glands just left of center are devoid of stroma. Scant fragments of crushed stroma are seen on the bottom right.
Yet another image to demonstrate the overall picture of scant cellularity and fragmentation.
Another patient with scant crushed stroma and small detached fragments of bland glandular epithelium.
Stromal crushing underneath epithelium in this setting is not indicative of true breakdown, as other features of breakdown are not present.
The tissue obtained during the biopsy in atrophy is typically scant. For the novice pathologist, being given a measly dab of mucoid material may incite feelings of anger and annoyance at the inept clinician. However, the experienced pathologist realizes that this scant material may be all there is -- and thus may be a clue to endometrial atrophy.
In an endometrial biopsy, one sees detached strips of surface endometrium and fragments of glands with very little stroma. The epithelial cells are cuboidal cells with small dark nuclei and little cytoplasm. If one were to receive a hysterectomy specimen or large fragments of tissue (quite unusual), the entire architecture could be seen. Small atrophic glands are haphazardly arranged in a fibrous and spindled stroma. The stroma may appear cellular because the stromal cells have lost most of their cytoplasm.
The cystic variant of atrophic endometrium consists of dilated and cystic glands lined by flattened epithelium. However, this variant is generally not appreciated in an endometrial biopsy specimen since the procedure of obtaining endometrial tissue (scraping or suction) disrupts and fragments the cystic glands.1,2
Atrophy is an important cause of post-menopausal bleeding and found in more than 25% of patients undergoing an endometrial biopsy. Atrophy results from an absence of estrogenic stimulation of the endometrium and thus is seen in postmenopausal women - either from normal aging, surgery, prior radiation, prior chemotherapy, or idiopathic premature ovarian failure. Endometrial atrophy can also be seen in women using continuous progestin birth control systems such as depo medroxy-progesterone acetate.
No treatment of endometrial atrophy is necessary once it has been diagnosed.
The condition is a safe reflection of hormonal status.
1 Robboy SJ, Anderson MC, Russell P. Pathology of the Female Reproductive Tract. London, UK: Churchill Livingstone; 2002: 257-9.
2 Mazur MT, Kurman RJ. Diagnosis of Endometrial Biopsies and Curettings. New York, NY: Springer; 2005: 113-5.