
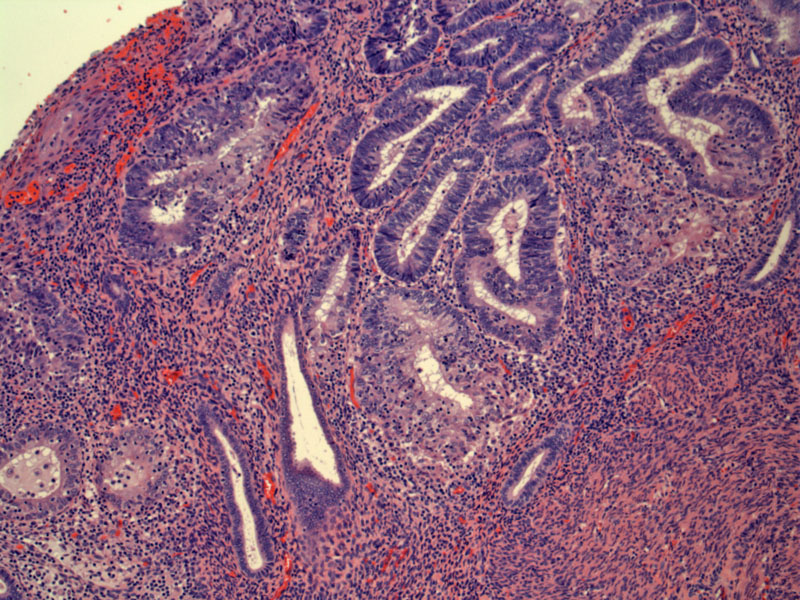
Neoplastic glands lined by enlarged hyperchromatic cells contain tumor infiltrating lymphocytes.
MLH-1 IHC shows absence of nuclear staining in the glands lined by the larger cells whereas the residual normal appearing glands lined by small cells show dark uniform staining
PMS-2 IHC shows a similar staining pattern, although overall staining is not as intense.
By contrast, MSH-2 as well as MSH-6 (not shown) both show staining in all the epithelial areas. Note that this is not abnormal. In a study of 45 MSI-H tumors, 22 cases demonstrated absent staining for MLH1 and PMS2 and positivity for MSH2 and MSH6 (Modica).
Review of the endometrial biopsy shows curretage of abundant material composed of a heterogeneous pattern of neoplasia. Some areas show the typical endometrioid pattern of carcinoma as in this field. Tumor heterogeneity may be a common feature in MSI-H tumors, however, some studies do not support this claim.
Other areas are more consistent with a malignant clear cell component. There are enlarged hyperchromatic nuclei within the clear cell sheet (left).
Another area consistent with a clear cell morphology -- high grade nuclear features can be appreciated.
Yet another area with serous features were seen.
Some endometrioid foci show mucinous metaplasia. Mucinous differentiation is another feature that is more frequently found in MSI-H tumors, however, some studies do not support this assertion.
Patients with hereditary nonpolyposis colorectal cancer (HNPCC), also known as Lynch syndrome, are predisposed to developing carcinomas, especially of the colon and endometrium. Cancers may also be seen in other organs of the GI tract including the stomach and pancreas, as well as reproductive organs such as the ovaries at much lower rates. The molecular basis of carcinogenesis is a germline mutation in one of the DNA mismatch repair genes (MSH1, MSH2, MSH6 or PMS2), leading to a high frequency of microsatellite instability when cells replicate. Tumors arising from DNA-mismatch repair are termed MSI-H (microsatellite instability - high frequency) tumors.
Note that sporadic tumors may also develop via this pathway -- for example, when methylation silences DNA mismatch-repair genes. Colorectal MSI-H tumors have been studied extensively, and endometrial MSI-H carcinomas have had less focus, however, recent data reveals numerous similarities between the two, not surprisingly.
Like colorectal MSI-H carcinomas, endometrial MSI-H carcinomas exhibit certain morphologic features such as tumor infiltrating lymphocytes, peritumoral lymphocytes, mucinous differentiation, tumor heterogeneity and medullary growth. In a study comparing 52 MSI-H endometrial carcinomas (as confirmed by PCR) with 50 non-MSI-H tumors, Shia and colleagues found that tumor infiltrating lymphocytes and peritumoral lymphocytes have significant predictive value in identifying MSI-H tumors (Shia).
In a study of 45 MSI-H endometrial carcinomas using IHC, Modica and colleagues found that the most common staining pattern was concurrent loss of MLH1 and PMS2 with positivity for MSH2 and MSH6. Although the authors found that interpretation of IHC was more problematic for MSI-H endometrial tumors when compared to MSI-H colorectal cancers, performing a panel of IHC markers for the DNA mismatch repair genes was helpful in supporting a diagnosis of mismatch repair related endometrial tumors (Modica).
Endometrial carcinoma is the most common carcinoma in women with HNPCC, with lifetime prevalences approaching 60%. MSI-H endometrial carcinomas usually occur in premenopausal women, and present with abnormal uterine bleeding. These carcinomas tend to be of the endometrioid type.
Uterine cancers are surgically staged with a total hysterectomy, bilateral salpingo-oophorectomy, pelvic washings, and pelvic and peri-aortic lymphadenectomy. Depending on degree of spread, patients may undergo vaginal cuff or whole pelvic radiation therapy.
There has been some evidence suggesting that patients with MSI-H tumors have improved prognosis compared to patients with non-MSI-H tumors and patients with sporadic MSI-H tumors. However, this assertion has been challenged by recent studies. Further investigation into MSI-H tumors will be necessary before we truly understand the behavior and prognosis for these tumors.
• Colon : Adenocarcinoma, Mismatch Repair Related
Modica I, Soslow RA, Black D et al. Utility of Immunohistochemistry in Predicting Microsatellite Instability in Endometrial Carcinoma. Am J Surg Pathol 2007;31:744-751.
Shia J, Black D, Hummer AJ et al. Routinely assessed morphological features correlate with microsatellite instability status in endometrial cancer. Human Pathology 2008:39;116-125.