
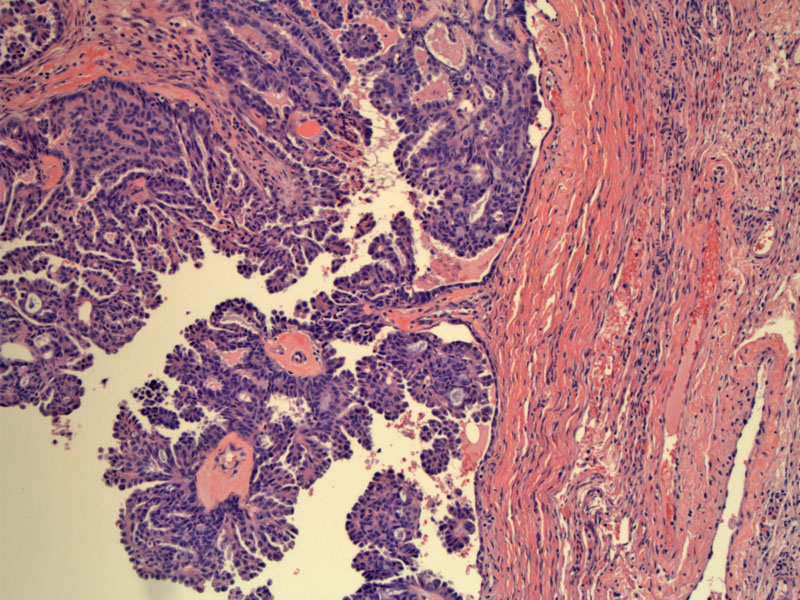
Here is the borderline serous tumor located on surface of ovary. Note the papillary growth with tufting of the epithelial cells.
This is the omentum with invasive implants. While noninvasive implants present themselves following between the septal lobulations of omental fat, the invasive type of implant grows into the fat, disregarding these natural planes.
The peritoneal wall shows involvement by tumor cell clusters consistent with a microinvasive implant. Clusters of neoplastic cells are singly infiltrating into the soft tissue.
Serous tumors of low malignant potential (S-LMP), otherwise known as serous borderline tumors, are accompanied by extra-ovarian implants of morphologically similar neoplasms. These implants are located on the peritoneal surfaces such as the serosa of surrounding organs and omentum. Implants are divided into invasive and non-invasive implants. The key difference between the two is the presence or absence of invasion and destruction of normal adjacent tissue.
Whereas non-invasive implants have a smooth and well-demarcated interface between the implant and surrounding tissue, invasive implants will destroy and infiltrate the peritoneal or omental soft tissue. Invasive implants are detected in approximately 5-10% of S-LMP cases -- however, this low number may be partly attributed to the difficulty in recognizing invasive implants and in distinguishing the difference between invasive implants from non-invasive implants, especially desmoplastic non-invasive implants.1,2
By definition, well-differentiated serous tumors featuring destructive stromal invasion are classified as low-grade serous carcinomas whereas those with either no stromal invasion or stromal microinvasion are classified as serous tumors of low malignant potential (S-LMP) (McKinney 2006).
The majority of S-LMP are clinically benign, but recurrences are not uncommon, and tumor related deaths occur. Progression to low-grade serous carcinoma is associated with more aggressive disease. Other features associated with recurrent and/or progressive disease include FIGO stage, invasive implants, microinvasion in the primary tumor. Generally these features occur in combination with one another (Longacre 2005).
♣ Invasive implants, micropapillary structures, ovarian stromal microinvasion and nodular lymph node aggregates are features that often occur in combination and are indicative of a more aggressive tumor.
• Ovary : Serous Borderline Tumor with Non-invasive Implants
• Ovary : Serous Borderline Tumor
• Ovary : Serous Borderline Tumor, Micropapillary Type
• Ovary : Serous Borderline Tumor with Non-invasive Implants
1 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 571-2.
2 Nucci MR, Oliva Esther. Gynecologic Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier: 2009; 401.
Longacre TA, McKenney JK, Tazelaar HD et al. Ovarian serous tumors of low malignant potential (borderline tumors): outcome-based study of 276 patients with long-term (> or =5-year) follow-up. Am J Surg Pathol 2005 Jun;29(6):707-23.