
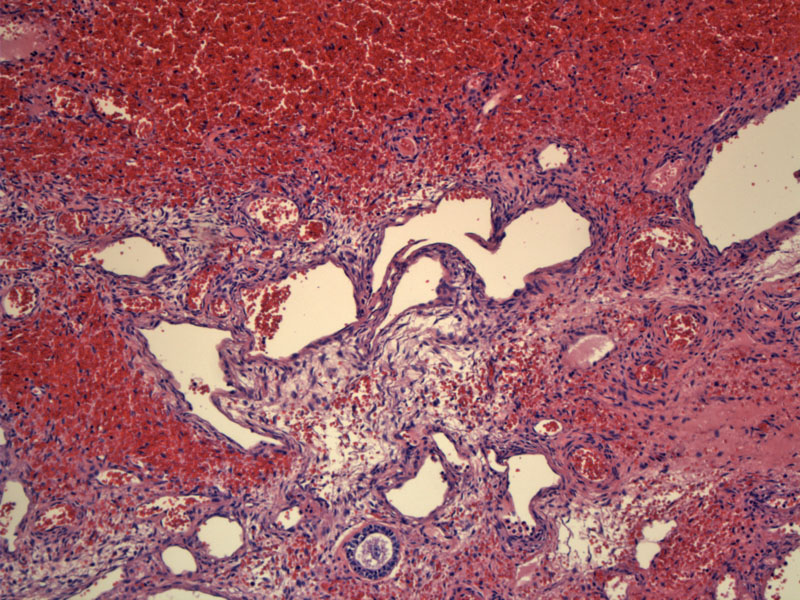
The ovarian parenchyma is edematous and engulfed by dissecting hemorrhage.
Most commonly, torsion is due to a coexisting tumor. Note the diffuse dissecting hemorrhage.
In this particular case, a mature teratoma was present. There is also hemorrhage within the stroma of the teratoma, seen best under the squamous lining (top).
Torsion occurs when the ovary rotates on its fibrovascular stalk, leading to strangulation of its blood supply and in severe cases, infarction of the ovary. In adults, the torsed ovary usually contains a cyst or tumor causes ovarian enlargement. Note that once an ovary reaches 6 cm in diameter, it lifts out of the pelvis, becoming freely mobile and susceptible to torsion. Furthermore, there is an increased risk of torsion during pregnancy as the ovaries are also more mobile during this time. 25% of cases of torsion occur in children and the ovary is frequently normal.1,2
Grossly, the ovary is enlarged, dark red and congested from the buildup of blood and fluid. One must carefully search for any underlying tumor or cyst that may be obscured by the blood. Most often, a benign tumor or cyst is the root cause of torsion, but a malignant tumor can also be found.1
Usually occurs in reproductive age women. Patients experience acute colicky abdominal pain, nausea and vomiting. In cases where an ovarian neoplasm is the cause of torsion, a palpable mass may be felt on physical exam. Patients with adnexal masses who are pregnant are at increased risk of torsion.
The standard therapy is oophorectomy. As many of these patients are young, more recently de-torsion and cystectomy has been attempted. Results have shown that following reperfusion, ovarian function may resume.
1 Crum CP, Lee KR. Diagnostic Gynecologic and Obstetric Pathology. Philadelphia, PA: Elsevier; 2006: 747-8.
2 Robboy SJ, Anderson MC, Russell P. Pathology of the Female Reproductive Tract. London, UK: Churchill Livingstone; 2002: 499-500.