
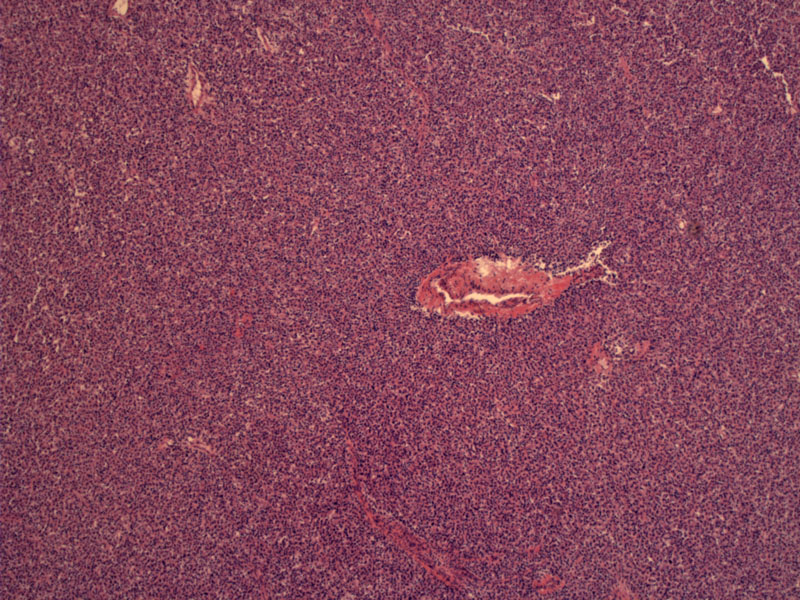
Solid sheets of chief cells expand the parathyroid with no intervening fat.
The cytoplasm of the neoplastic cells varies from lightly-tinged and granular to eosinophilic (oxyphilic) in appearance. The transitions can be abrupt, or the two population can be more intermingled randomly.
This is a less frequently encountered pattern -- polarized parathyroid cells with basally situated nuclei line up, producing a pseudopapillary architecture.
Beta-hcg shows mild to moderate distinct cytoplasmic staining in a minority of cells. Yes, interestingly, parathyroid neoplasms have been show to be focally immunoreactive with beta and alpha subunits of human chorionic gonadotrophin (Carlinfante). In fact, urinary HCG levels may be useful in distinguishing between parathyroid hyperplasia/adenoma and parathyroid carcinoma (Rubin).
Hyperparathyroidism can be primary, secondary and tertiary. Primary hyperparathyroidism is further divided by etiology: adenoma (75%-80%), hyperplasia (10%-15%), parathyroid carcinoma (<5%)(Kumar, Fletcher). Secondary hyperparathyroidism is usually secondary to chronic renal insufficiency. Tertiary hyperparthyroidism is autonomous hyperfunction of the parathyroid glands as a result of long-standing secondary hyperparthyroidism.
Most (95%) cases of primary hyperparathyroidism are sporadic, however, the remaining 5% associated with familial syndromes provide unique insight into molecular mechanisms of oncogeneis and thus, are heavily tested by the boards.
Familial syndromes associated with parathyroid hyperplasia and adenomas include: MEN type I, MEN type IIA, familial hypocalciuric hypercalemia (FHH), hyperparthyroidisim-jaw tumor syndrome.
FHH is a autosomal-dominant disorder in which the CASR (calcium-sensing receptor) on chromosome 3q is mutated. Thus, there is decreased sensitivity to extracellular calcium, leading to hyperparathyroidism. CASR mutations are not found on sporadic tumors. Individuals with homozygous mutations of CASR present with severe hyperparathyroidism as neonates (Kumar).
In hyperparathyroidism-jaw tumor syndrome, parathyroid adenomas or carcinomas (not parathyroid hyperplasia) is seen along with fibro-osseous lesions of the jaw as well as kidney tumors. It is an autosomal dominant disorder due to mutations of the HRPT2 gene on chromosome 1q25-31. It has a higher rate of parathyroid carcinoma (10-15%) compared to MEN I or MEN IIa (Fletcher).
In parathyroid hyperplasia, all four glands are involved, but in some instances, only one or two glands are hyperplasia and distinguishing between hyperplasia and adenoma can be very difficult (Kumar). Stromal fat is seen in normal parathyroid tissue but conspicuously absent in parathyroid hyperplasia and parathyroid adenoma.
Primary hyperparathyroidism is one of the major causes of hypercalcemia. It usually affects adults (age 50 or older) with a predilection for women (F:M ratio of 3:1)(Kumar). Symptoms of hypercalcemia include polyuria, polydipsia, mental disturbance, renal stones ("groans, moans and psychiatric overtones"). Hyperparathyroid disease of the bone can occur in these instances as well.
Parathetically, some tumors (e.g. SCC of the lung, renal cell carcinoma) can elaborate parathyroid hormone-related peptide and thus, lead to hypercalcemia (Fletcher). In these instances, the levels of PTH should be low (due to negative feedback), but PTH-rP will be elevated.
• Parathyroid : Parathyroid Adenoma
Carlinfante G, Lampugnani R, Azzoni C, Aprile MR, Brandi ML, Bordi C. Expression of the alpha- and beta-subunits of human chorionic gonadotropin by subsets of parathyroid cells in states of hyperparathyroidism. J Pathol. 1998 Aug;185(4):389-93.
Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 1080-6.
Kumar V, Abbas AK, Fausto N. Robbins and Cotran Pathologic Basis of Disease. 7th Ed. Philadelphia, PA: Elsevier; 2005: 1184-6.
Rubin MR, Bilezikian JP, Birken S, Silverberg SJ. Human chorionic gonadotropin measurements in parathyroid carcinoma. Eur J Endocrinol. 2008 Oct;159(4):469-74. Epub 2008 Jul 14.