
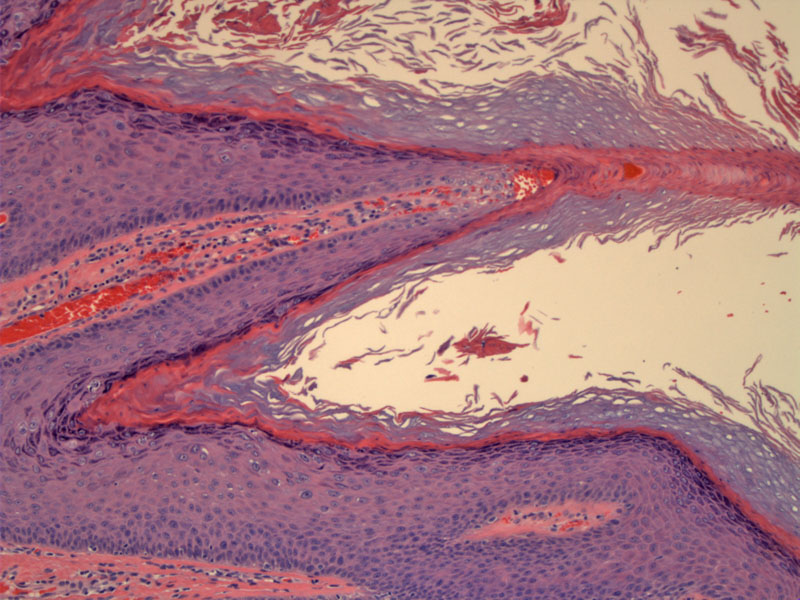
Condylomata is characterized by papillomatosis, acanthosis and parakeratosis. The undulating and thickened folds of epithelium are supported by a fibrovascular cores. The basal layer is largely unaffected (minimal cell enlargement or pleomorphism) and surface maturation is retained. Prominent papillary 'church spires' (papillomatosis) with delicate mounting parakeratosis (abnormal maturation with retention of nuclei) is illustrated here.
A distinctive feature of condylomata is the viropathic change (koilocytosis) seen in the superficial or intermediate cell layers. Hypergranulosis with nuclear atypia can be appreciated in the superficial layer of the epithelium.
Koilocytes are cells with enlarged, wrinkled, 'raisinoid' hyperchromatic nuclei surrounded by a perinuclear halo. Binucleate forms are not uncommon.
The tip of this papillary projection shows viropathic change with overlying parakeratosis.
Condyloma acuminata (genital warts) are sexually transmitted and over 80% are associated with HPV type 6 or 11. In contrast, VIN (vulvar intraepithelial neoplasia) is associated with high risks HPV types.1
Of note, in VIN lesions, grade I VIN exhibits dysplasia confined to the lower one-third of the epithelium. In grade II VIN, the dysplasia extends to the lower two-thirds of the epithelium. This is in contrast to condyloma acuminata where the abnormality is seen in the surface layer.
In some instances, the lesion exhibits acanthosis and papillomatosis, but koilocytic change is not obvious -- nonetheless, these lesions called 'fibroepithelial papillomas' are strongly associated with HPV and are considered a variant of condyloma acuminatum. Yet another variation resembles seborrheic keratosis as demonstrated by a proliferation of basaloid cells, horn cysts and absent koilocytosis -- studies again demonstrate a strong association of HPV type 6 in these unusual condylomata.2
Condylomata acuminata, commonly referred to by clinicians as anogenital warts, can occur in cervix, anus, vulva and vagina. Can present with itching, burning, bleeding and vaginal discharge. Lesions are velvety in texture and can range from small and asymptomatic to large obstructive mats that can interfere with intercourse and vaginal delivery. Application of acetic acid causes the lesion to turn white.
Various treatment modalities are available. Applying chemicals is preferred for smaller lesions. Tricholoroacetic acid is considered a good initial approach, however, repeated applications are often necessary. Podophyllin is also a good topic medicine, however, it cannot be applied on mucosal surfaces such as the vagina. Podophyllin is also contraindicated in pregnancy. Cyrotherapy with liquid nitrogen is another commonly employed treatment modality.
For larger lesions or in situations when medical therapy is not effective, surgical removal with laser ablation or excision may be necessary.
Condyloma acuminatum is associated with low-risk HPV subtypes 6 and 11. All treatment modalities have high recurrence risks. Conditions such as AIDS and pregnancy are associated with rapid progression of lesions. It is also important to note that while benign HPV subtypes cause condyloma accuminatum, they are often present in association with the high risk HPV subtypes that may cause cancer.
• Cervix : Condyloma Acuminata
1 Mills SE, ed. Sternberg's Diagnostic Surgical Pathology. 5th ed. Philadelphia, PA: Lippincoott Williams & Wilkins; 2009: 2100-2107.
2 Crum CP, Lee KR. Diagnostic Gynecologic and Obstetric Pathology. Philadelphia, PA: Elsevier; 2006: 112-5.