
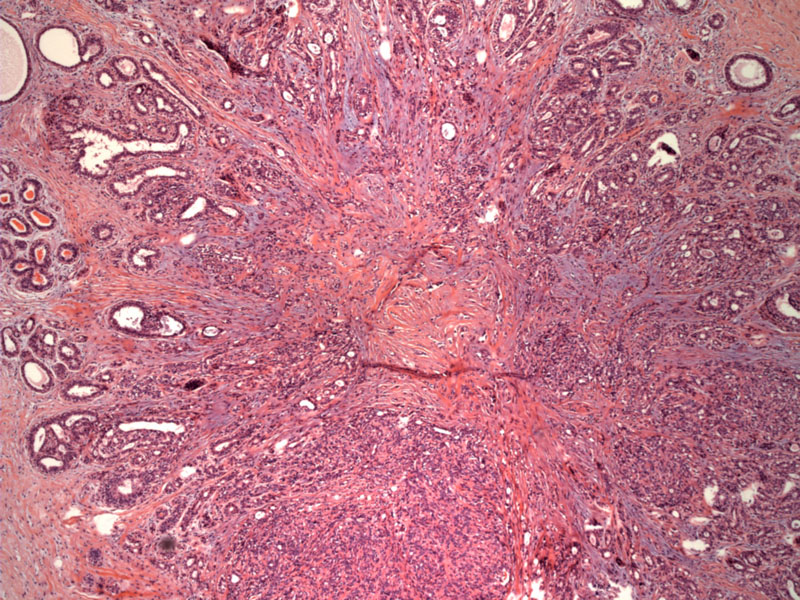
A radial scar is composed of a central sclerotic core of acellular fibrous tissue and elastin deposits. Entrapped ductules in the core have an intact myoepithelial layer, an important distinguishing feature from tubular carcinoma. Glands entrapped in the central fibroelastic core tend to be compressed and angulated, whereas the lumens of the glands become more visible as you move outward from the central core. Similar to sclerosing adenosis, the architectural features of radial scars are best viewed at low power.
Along the periphery, there is a radial proliferation of distorted ducts and lobules exhibiting benign proliferative changes as sclerosing adenosis, ductal hyperplasia, cyst formation, and papillomatosis.
A radial scar is not a true scar as it is unrelated to any prior trauma or surgery, rather, the term is a morphologic description. The lesion consists of a fibroelastic central core, which can be hyalinized and sclerotic (scar-like), from which there are radiating "bands" of ducts and lobules. These ducts and lobules often exhibit various proliferative changes, the most common being duct hyperplasia, sclerosing adenosis and cysts.1
Other synonymous terms include complex sclerosing lesions or radial sclerosing lesions (preferred by Rosen).
Their most important clinical feature is their propensity for associated microcalcification and mimicry of malignancy. The stellate, sclerotic gross appearance of this lesion can be grossly indistinguishable from carcinoma.
Microscopically, complex sclerosing lesions can be confused with tubular carcinomas. In this latter instance, staining the myoepithelial cells (using p53 and smooth muscle myosin markers) may be helpful.
1 Rosen PP. Rosen's Breast Pathology. 3rd Ed. Philadelphia: Lippincott Williams & Wilkins; 2009:100-4.
2 O'Malley FP, Pinder SE. Breast Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elvesier; 2006: 90-6.