
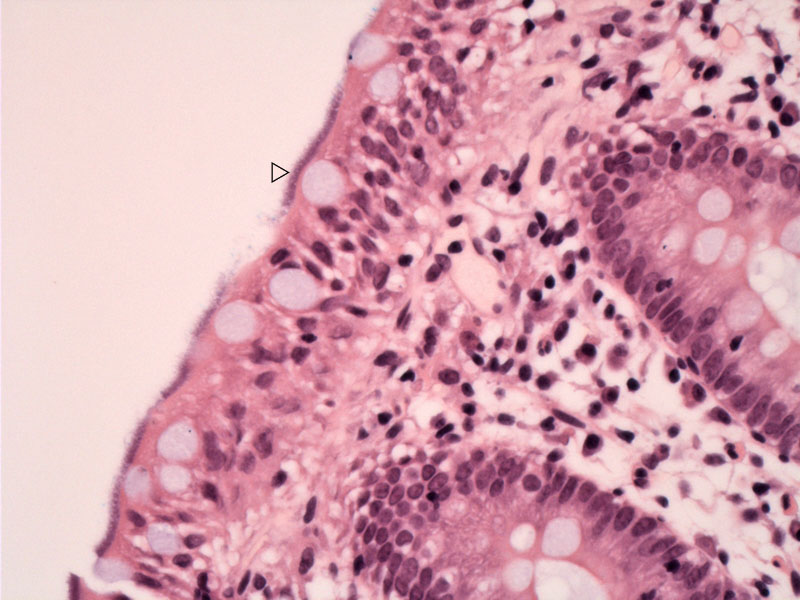
Note the blue fuzzy layer along luminal surface of the enterocytes. No inflammatory reaction is present.
The corresponding Warthin Starry stain shows intense black staining of the organisms. You may be able to detect the spirochetes in the goblet cell if you look closely.
Another image shows the thickened layer along the lumen and some fuzzy rimming of the edge
Another case emphasizes that the architecture remains intact and there is no inflammatory response.
Intestinal spirochetosis is primary seen in homosexual men although it has been described in a variety of situations. The prevalence of spirochetosis in humans ranges from 2.5 to 16% in Western countries (Lindboe).
Patients usually have diarrhea as the cause of the colonoscopic biopsy, but it is not always clear that the spirochetosis is etiologically related as the organism may be detected following symptom resolution. However, other studies do demonstrate sustained clinical recovery after spontaneous or drug-induced spirochetal disappearance in individuals with chronic diarrhea, suggesting that perhaps in some, intestinal spirochetosis may truly play a pathogenic role in this condition (Esteve; Calderaro). Any level of the colon may be involved and it may be focal.
Asymptomatic patients are usually not treated. Symptomatic and high-risk groups often will receive an active treatment with metronidazole.
Lindboe CF. The prevalence of human intestinal spirochetosis in Norway. Anim Health Res Rev. 2001 Jun;2(1):117-9.
Esteve M. et al. Intestinal spirochetosis and chronic watery diarrhea: clinical and histological response to treatment and long-term follow up. J Gastroenterol Hepatol. 2006 Aug;21(8):1326-33.
Calderaro A. et al. Infective colitis associated with human intestinal spirochetosis. J Gastroenterol Hepatol. 2007 Nov;22(11):1772-9.