
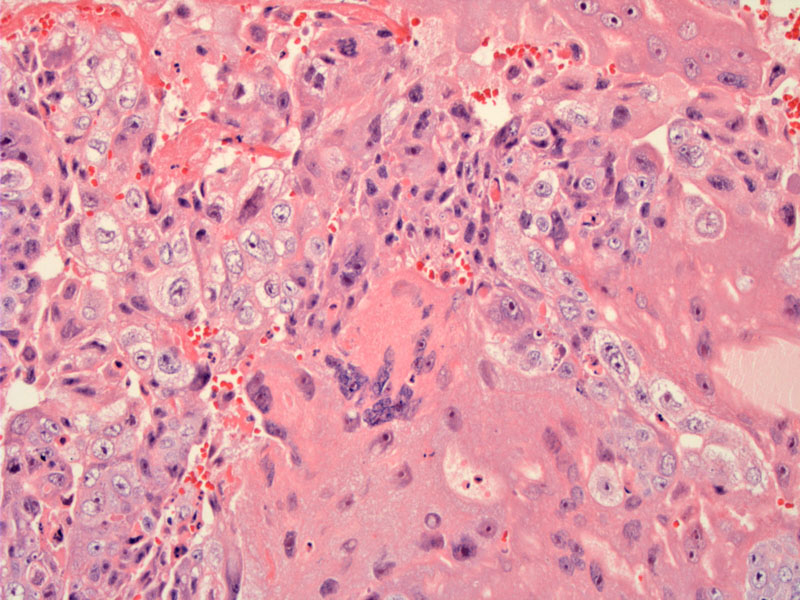
These tumors show an admixture of syncytiotrophoblasts, cytotrophoblasts, extravillous trophobasts with hemorrhage, necrosis and areas of vascular invasion. Here you can see that the malignant trophoblasts demonstrate prominent cytologic atypia. The cytotrophoblasts are enveloped by syncytiotrophoblasts (multi-nucleated cells which elaborate HCG).
Benign trophoblastic tissue (left) is contrasted with malignant trophoblastic cells with prominent cytologic atypia (right).
An intimate admixture of trophoblastic cells (cytotrophoblasts and syncytiotrophoblasts) is seen here. Grading is not employed with choriocarcinoma as all choriocarcinomas are aggressive and behave similarly.
Another area demonstrates an almost spindled confluent growth of the neoplastic cells.
A second case, obtained from an endometrial biopsy, shows abundant hemorrhage and fibrin deposition -- common features in choriocarcinoma.
Malignant cells with enlarged pleomorphic nuclei is seen on the left and some benign cells are seen on the right.
A third case, also from an endometrial biopsy, shows benign decidualized cells and malignant trophoblasts (right and left, respectively) -- replete with extensive hemorrhage and inflammation.
From yet another case, this is a hysterectomy showing the tumor interface. Note the myometrial fibers (on the left) heavily infiltrated by chronic inflammatory cells.
Here is a more convincing area of invasion, with pleomorphic trophoblastic cells dissecting through the muscle fibers (spindled pink cells) of the myometrium.
Gestational choriocarcinoma is a malignant proliferation of trophoblastic cells derived from a normal or abnormal pregnancy. In the US, the incidence is approximately 1 in 20,000 or 30,000 pregnancies. Of interest, it is much more common in some African countries such as Nigeria, where the incidence in some areas is as high as 1 in 2500 pregnancies!1
Half of all cases are preceded by a molar pregnancy, 25% occur in abortions, 22.5% occur in normal pregnancies and 2.5% occur in ectopic pregnancies.2 Aproximately 1 in 40 hydatiform moles will result in a choriocarcinoma, while in contrast, only 1 in 250,000 normal pregnancies will give rise to a choriocarcinoma.
Grossly, a mass that is variably yellow-white, fleshy and hemorrhagic is seen in the uterus. Due to its propensity to grow rapidly, areas of infarction, hemorrhage and necrosis are common. On cross section, the tumor will be seen invading the myometrium, and sometimes, extending into the uterine serosa and adjacent structures.
Syncytiotrophoblasts are strongly positive for hCG and weakly reactive with hPL (human placental lactogen). All trophoblastic cells stain strongly with cytokeratins. This IHC profile may be helpful in distinguishing choriocarcinoma from placental site trophoblastic tumor (PSTT). PSTT will stain strongly with hPL. Furthermore, in PSTT, the predominate cell are monomorphic intermediate trophoblasts with lesser amounts of syncytiotrophoblasts.2
Most cases arise in the uterus, however, choriocarcinoma can be found outside of the uterus in ectopic pregancies. Women will complain of spotting and discharge, but a mass is usually not palpable. The neoplasmsis usually discovered on an endometrial biopsy.
The tumor can occur during the pregnancy or several months after pregnancy -- intervals as long as 14 years have been reported!2 Radiographs often reveal metastatic lesions in the lung and bones, leading to symptoms of hemoptysis and neurologic derangments. hCG levels are highly elevated. Exceptionally, the tumor may produce very little hormone (usually as a result of extensive necrosis).
After determining the presence or absence of metastases, patients are stratified into high and low risk groups depending on a variety of factors. Non-metastatic and low risk groups may experience cure with single agent chemotherapy (typically methotrexate), while multi-agent chemotherapy (etoposide, methotrexate, actinomycin-D, cyclophosphamide, vincristine) is employed in high risk patients. Radiation may be added to treat brain metastases. Hysterectomy may have a role in patients not desiring fertility preservation. HCG levels are used as markers for treatment response and recurrance.
Widespread and rapid metastasis is characteristic of this tumor -- most frequent locations include lungs (50%), vagina (30-40%), brain and liver. Fortunately, remission rates using chemotherapy are upwards of 100%. Of note, nongestational choriocarcinoma are much more resistant to chemotherapy.
♥ hCG is highly elevated
♥ Widely and rapidly metastatic
♥ Often associated with hydatidiform moles
♥ Exquisitely sensitive to chemotherapy (fortunately)
• Ovary : Choriocarcinoma, nongestational
• Ovary : Choriocarcinoma, nongestational
• Placenta : Placental Site Trophoblastic Tumor
1 Kumar V, Abbas AK, Fausto N. Robbins and Cotran Pathologic Basis of Disease. 7th Ed. Philadelphia, PA: Elsevier; 2005: 1113-4.
2 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 677-678.