
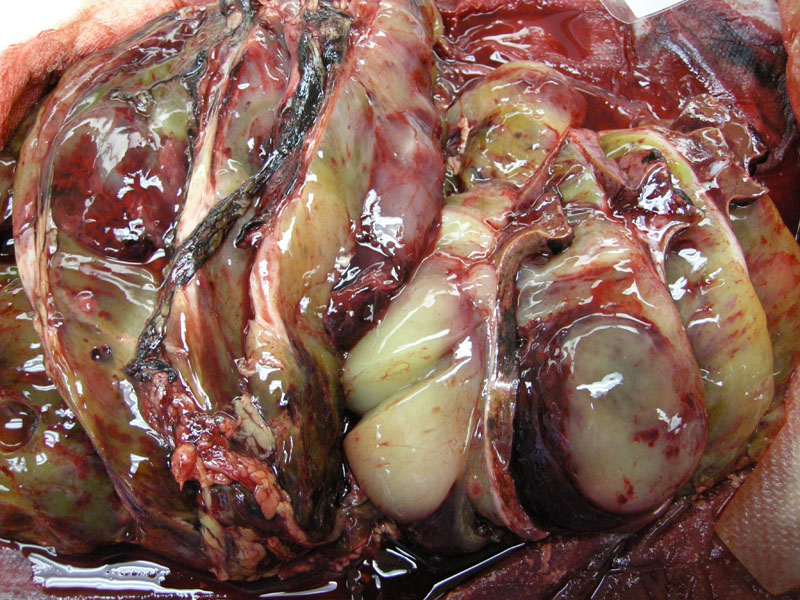
The gross specimen demonstrates a large, fleshy and gelatinous tumor. Hemorrhage, necrosis and cystic degeneration are common findings.
Stellate and spindled tumor cells are set in a mxyoid stroma.
Large atypical tumors cells, multinucleated cells and mitotic figures are frequently throughout the tumor.
Cytoplasmic hyaline globules that are PAS positive and diastase resistant are highly characteristic and maybe represent alpha1-antitrypisin uptake by tumor cells.2
A more cellular area is seen with epithelioid neoplastic cells containing round nuclei -- note the open vesicular chromatin.
The hyaline globules (cytoplasmic and stromal) stain with alpha1-antitrypsin.
Keratin AE1/3 (pan-keratin stain) demonstrates focal positivity.
Undifferentiated embryonal sarcoma is a rare neoplasm of childhood, typically occurring between ages 6-10. Older terms include malignant mesenchymoma, fibromyxosarcoma and rhabdomyosarcoma of the liver.
Grossly, the tumor is large (approximately 30 cm in diameter), soft with a shiny gelatinous surface. Degenerative changes such as necrosis, hemorrhage and cystic degeneration are common. Although the tumor may appear well-circumscribed, there is usually tumor infiltration beyond the pseudocapsule.
Microscopically, there is a mixture of atypical spindle and stellate cells with ill-defined cell borders embedded in a myxoid stroma. The neoplastic cells may contain PAS-D positive cytoplasmic globules -- these globules may also be present in the stroma and may be attributed to alpha1-antitrypsin (Iacbuzio). Large bizarre cells with hyperchromatic nuclei and multinucleated tumor cells are scattered throughout and mitotic activity is brisk. Extramedullary hematopoiesis is often identified, and entrapped hepatocytes and ductules are often seen on the periphery (Fletcher).
IHC studies of 14 primary and 2 recurrent embryonal sarcomas demonstrated that tumors are strongly positive for vimentin and the cytoplasmic globules stain with alpha1-antitrypsin. Focal positivity with keratins, desmin and SMA can be seen. The tumor is generally negative for HepPar1, AFP, S-100, HMB45 and CD34 (Zheng).
Do not confuse undifferentiated embryonal sarcoma with embryonal rhabdomyosarcoma, which arise from the major bile ducts at the hilum. Embryonal rhabdomyosarcoma affects younger children (<5 years) and presents with jaundice, fever and weight loss. Grossly, a botryoid (grape-like) gelatinous mass is seen in the lumen of common or left/right bile ducts. Microscopically, there is a zone of hypercellulary (cambium layer) and spindle cells in a myxoid stroma. Typical rhabdomyoblasts with cross-striations are rarely seen (Stocker, Cheng).
In terms of IHC reactivity, embryonal rhabdomyosarcoma are positive for desmin, myoblogin and myosin, demonstrating increased differentiation toward muscle, whereas undifferentiated embryonal sarcoma are more pluripotent with multiple lines of differentiation (Zheng).
Most commonly occurs between age 6-10 with equal gender distribution. Typically presents with abdominal pain or an abdominal mass. Serum AFP (consistently found in hepatoblastoma and hepatocellular) is not present in this tumor.
Surgical resection with combination chemotherapy has increased survival, although prognosis is still poor. Adjuvant pre-operative and post-operative chemotherapy appear to improve outcome.
Poor -- In a review 67 cases over 15 years, 73% of patients had died (Stocker). Complete surgical resection provides the best outcome, however, this is difficult since the tumors are often large on presentation. Lung, pleura and peritoneum are favored sites of metastatis.
Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 442-3.
Iacobuzio-Donahue CA, Montgomery EA. Gastrointestinal and Liver Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier; 2005: 622-4.
Stocker JT. Hepatic tumors in children. Clin Liver Dis. 2001 Feb;5(1):259-81, viii-ix.
Zheng JM, Tao X, Xu AM et al. Primary and recurrent embryonal sarcoma of the liver: clinicopathological and immunohistochemical analysis. Histopathology. 2007 Aug;51(2):195-203. Epub 2007 Jun 15.