
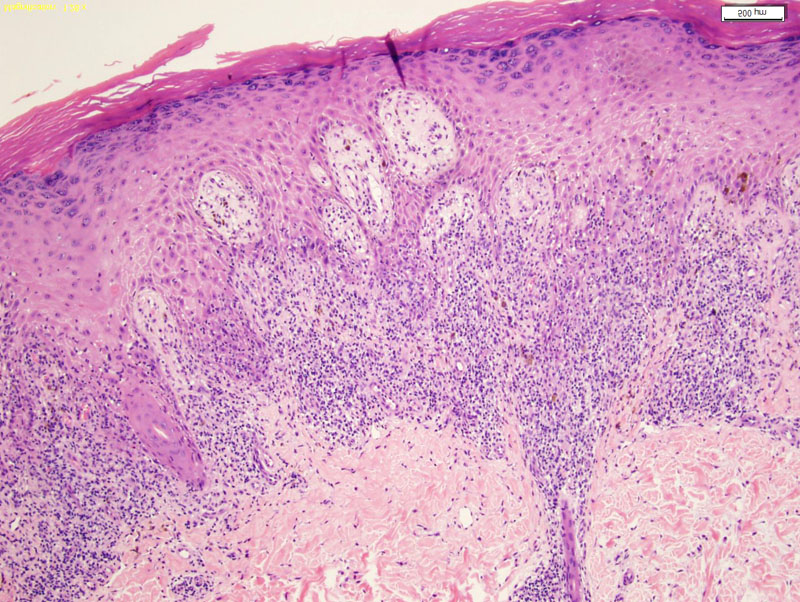
There is a dense lichenoid infiltrate of lymphocytes which obscures the dermal-epidermal junction. The overlying epidermis demonstrates hypergranulosis and compact hyperkeratosis.
The rete ridges have a jagged or sawtooth outline.
Other features of LP include melanin incontinence and hydropic degeneration (in which there are vacuolar spaces between the dermal-epidermal junction). The latter feature is a bit subtle here.
Lichen planus (LP) may be an immune reaction to a drug or in ~10% of cases, hepatitis C infection.
LP is the prototypical example of the lichenoid pattern of interface dermatitis. Interface dermatitis can be divided into lichenoid and vacuolar patterns. A lichenoid pattern is composed of: (1) a bandlike infiltrate at the dermal-epidermal junction (2) presence of "colloid bodies", which are necrotic keratinocytes in the basal layer (3) pigment incontinence.
The other type of interface dermatitis is the vacuolar pattern which exhibits many of the same features as the lichenoid pattern, however, vacuolar dermatitis is characterized by intracytoplasmic vacuoles within the basal keratinocytes. Conditions seen in the vacuolar pattern include lupus, dermatomyositis, PLEVA, lymphmatoid papulosis and acute GVHD (Sternberg).
Lichen planus is characterized by the five "Ps": polygonal, planar, pruritic, purplish and papules. They tend to be located on the wrist, lower back, ankles and in some instances, may affect the mouth and genitals. On physical exam, there are delicate white lines called "Wickham's striae" over the surface of the papules. These lesions can be very itchy.
Onset may be sudden or gradual. Recurrences may happen for years, althouth in the majority of cases, lesions are self-limited and resolve within months to years.
Asymptomatic cases do not require treatment. Topical steroids may be used in mild cases, with oral predinose possibly with UV light, for more severe cases.
→There is an association between lichen planus and hepatitis C virus and primary biliary cirrhosis.
→Histologic features of LP include a lichenoid infiltrate, irregular acanthosis, hyperkeratosis, hypergranulosis and colloid boides close to the basement membrane.
Rapini RP.Practical Dermatopathology. Philadelphia, PA: Elsevier; 2005: 53-6.
Mills SE, ed. Sternberg's Diagnostic Surgical Pathology.4th Ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2004: 9.