
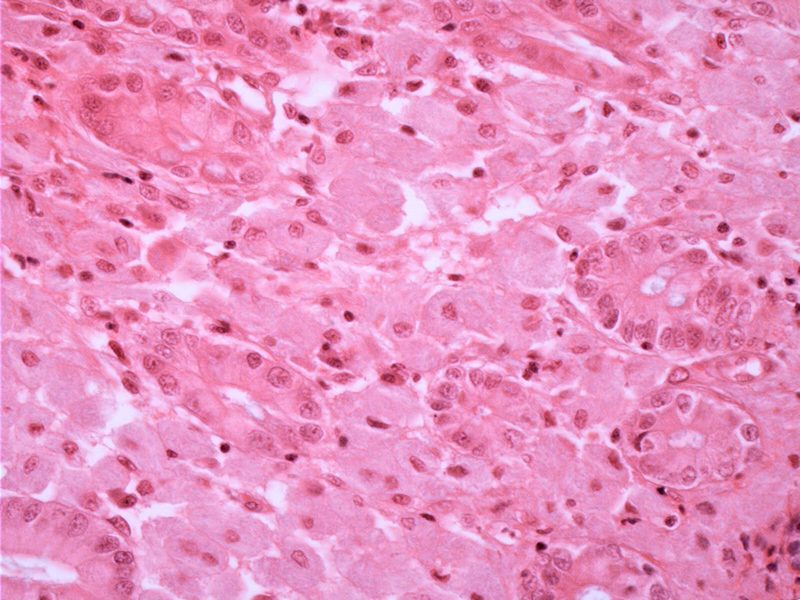
Sheets of pale staining macrophages expand the lamina propria between the glands. The overall inflammation is minimal -- occasionally poorly formed epithelioid granulomas may be seen. Grossly yellow-whitish nodules may be seen, and the mucosa may appear edematous, with patchy involvement.
Mycobacterial organisms are innumerable, filling the cytoplasm of the macrophages. MAI are beaded organisms measuring 4-6um in length, and are not distinguishable by their shape from other mycobacterial organisms. However, this intracellular location and sometimes stacked arranged is distinctive.
With the introduction of antimicrobial prophylaxis and highly active antiretroviral therapy (HAART), the incidence of disseminated MAI infection has dramatically declined.
Common presenting symptoms include diarrhea, fever, weight loss, and abdominal pain. Within the GI tract, a number of lesions may be seen including gastric ulceration, enterocolitis, enteric fistulas, intra-abdominal abscess, and hemorrhage. In the 55 reported cases of MAC infection of the GI tract, the duodenum (76%) was the most common site, followed by the rectum (24%), the ileum (6%), the colon (4%), the esophagus (4%), the jejunum (2%), and the stomach (2%) (Cinti)
Treatment for disseminated MAC in AIDS patients whos CD4 counts are <200/mm3 involves rifabutin, clarithromycin, and azithromycin administered together.
• Small Intestines : Histoplasmosis
S.K. Cinti, D.R. Kaul, P.E. Sax, L.R. Crane and P.H. Kazanjian, Recurrence of Mycobacterium avium infection in patients receiving highly active antiretroviral therapy and antimycobacterial agents, Clin Infect Dis 30 (2000), pp. 511–514.