
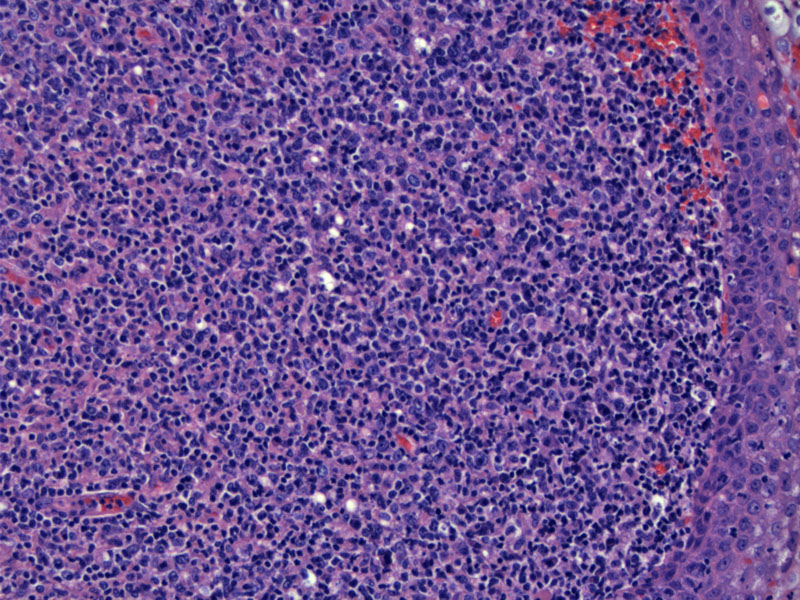
The squamous mucosa of the palantine tonsil remains intact, with a lymphoid population undermining it. Image
Some larger cells with vesicular chromatin are present.
Ki-67 is extremely high in this diffuse large B cell lymphoma, but not quite 100% (100% Ki-67 positivity would make you worry about Burkitt!)
CD20 is expressed throughout the malignant cell population. Rituximab (Anti-CD20) is often employed as a treatment modality in these patients.
Bcl-6 is the most frequently translocated and/or mutated gene in diffuse large B cell lymphoma (up to 30% of cases). Some but not all nuclei are staining for this.
Of all head and neck sites, the tonsils are the most common site of involvement by malignant lymphoma. The tonsils are included in Waldeyer ring, which refers to the circular band of lymphoid tissues located at the opening of the upper aerodigestive tract, consisting of the nasopharynx, oropharynx, tonsil, and base of the tongue.
Although relatively rare in Western countries, Waldeyer ring is the commonly involved site of lymphoma in Asia and Mexico and accounts for 25% of all non-Hodgkin's cases in China 1 . Large B cell lymphoma is the most common subtype affecting the tonsil region. A minority are EBV associated, a percentage that varies in different studies, which perhaps is related to the number of HIV patients included. A small percentage arises out of a pre-existing MALT lymphoma, CLL/SLL, or follicular lymphoma.
The immunohistochemical profile of DLBCL shows positivity for B cell markers (i.e. CD20 and CD79a) and a Ki-67 proliferation index of ~90%. EBER in-situ hybridization is also a useful stain to determine if the lymphoma is due to EBV infection (though it is more frequently positive in Burkitt lymphoma). See the 'prognosis' section for utility of Bcl6/CD10 and MUM1.
Don't forget about ruling out other entities! One of the most important entities to rule out is Burkitt lymphoma, which is also a medium to large cell lymphoma with a high proliferative rate. CD43 and Bcl2 are helpful to distinguish these two entities, as CD43 is positive in Burkitts, and negative in DLBCL while Bcl2 is positive in DLBCL, but negative in Burkitt. Finally, a negative cyclin D1 will help you sleep better, knowing you covered your bases, looking for a mantle cell lymphoma.
The molecular features of DLBCL vary, but the most common abnormality (30% of cases) occurs in the 3q27 region involving the Bcl6 gene. Translocations also occur, such as t(14;18) - the translocation resulting in activation of the Bcl2 gene and associated with follicular lymphoma. Also, just to make things complicated, t(8;14) - characteristic of Burkitt lymphoma - can also be present. There is controversy concerning what one should call a DLBCL with the myc rearrangement and other translocations or molecular abnormalities, but the WHO 2008 recommends 'B-cell lymphoma, unclassified with features intermdiate between diffuse large B-cell lymphoma and Burkitt lymphoma'. 2
Treatment includes combined chemotherapy [CHOP regimen (cyclophosphamide, doxorubicin, vincristine, and prednisolone)] and involved field radiation therapy. For those presenting with advanced stage and CD-20 positivity, rituximab plus CHOP (R-CHOP) has been established as the new standard systematic therapy.
5 year survival rates for those involving any area of Waldeyer ring is approximately 75%1 . Overall, patients have similar response rates and clinical outcomes to those with diffuse large B cell lymphoma which is nodal based.
Some studies have shown that immunohistochemical subtyping to determine the probable the cell of origin (ie germinal center cell vs. activated B cell) can provide prognostic information 3 . This can be accomplished with CD10, Bcl6 and MUM1. All CD10+ and CD10-/Bcl6+/MUM1- DLBCLs are regarded as germinal center cell subtype and all others are activated B cell subtype. Gene expression profiling has shown that the germinal center cell subtype has a better prognosis with a 5 year survival of 50-60% while the activated B-cell subtype has a 5 year survival of 15-30%.2 Since the immunohistochemical subtyping of these lymphomas does not perfectly correlate with the gene expression profiling, therapies are not yet based on these immunohistochemical profiles.
1. Qi SN, et al. Diffuse large B-cell lymphoma: clinical characterization and prognosis of Waldeyer ring versus lymph node presentation. Cancer. 2009 Nov 1;115(21):4980-9.
2. Swerdlow SH, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H, Thiele J, Vardiman J, WHO Classification of Hematopoeitic and Lymphoid Tissues 4th Ed. WHO Press; 2008: pp 356-357.
3. Colomo L et al. Clinical impact of the differentiation profile assessed by immunophenotyping in patients with diffuse large B-cell lymphoma. Blood 101:78-84.