
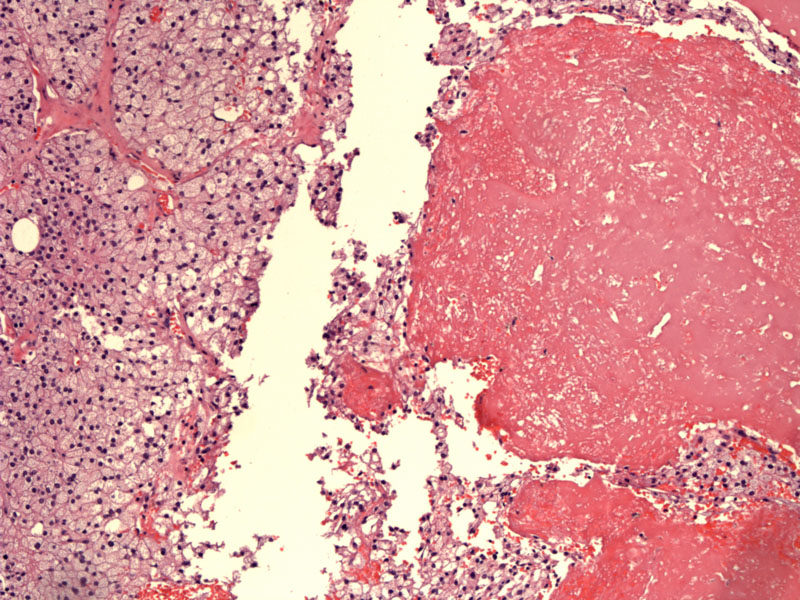
Vaguely lobular nests of neoplastic cells with pale foamy cytoplasm is seen on the left. Secondary hemorrhage is see on the right.
Clusters and cords of neoplastic cells are seen in background of eosinophilic and hyalinzed matrix. There may be some mild cytologic atypia, but it is usually not confluent and not prominent.
Normal adrenal cortical cells are highly similar, seen here for comparison.
A different example shows an admixture of clear cells and eosinophilic granular cells, with focal nuclear hyperchromasia and pleomorphism. Focal cytologic atypia is commonly seen in adenomas and is not used as feature to distinguish between cortical adenomas and cortical carcinomas.
80% of cortical adenomas are discovered incidentally. In most instances, they are nonfunctional tumors, meaning that they do not secrete steroid hormones. Functional cortical adenomas, on the other hand, can cause any of the three forms of hyperadrenalism, depending on which of the three steroid hormones are overproduced.
The vast majority of cortical adenomas are small (2cm), unilateral and solitary well-circumscribed lesions. Neoplastic cells generally look similar to those of the cells composing the normal adrenal cortex, but may be more pleomorphic. The cytoplasm of the neoplastic cells can range from clear (resembling zona fasciculata) to eosinophilic (resembling zona reticularis). Common architectural patterns include alveolar nests or short trabeculae. Degenerative and secondary features such as hemorrhage, fibrosis, dystrophic calcification and metaplastic bone formation are not uncommon.
Hyperaldosteronism (excess of aldosterone) is the most common manifestation, followed by Cushing syndrome (excess of cortisol). Virilization or feminization (excess of sex hormones) is rare, but is an ominous sign and strongly associated with malignancy.
Adenomas producing corticosteroids (Cushing syndrome):
- Grossly, the adenoma is yellow with brown mottling
- The uninvolved cortex of adrenal gland adjacent to the adenoma and the contralateral adrenal gland will be atrophic due to negative feedback.
- Microscopically, the tumor cells resemble that of the zona fasciculata (which as you may remember, make corticosteroids). Zona fasiculata cells will have abundant, foamy, lipid-filled cytoplasm. There may also be admixed cells with eosinophilic cytoplasm resembling zona reticularis cells.
Adenomas producing aldosterone (Conn syndrome):
- Grossly, the adenoma is usually less than 3cm in diameter and is bright canary yellow.
- Microscopically, the cells resemble those of zona glomerulosa (small darkly-staining round centrally placed nuclei with pale amphophilic cytoplasm) or zona fasciculata or a hybrid of the two forms.
- A unique cytoplasmic inclusion called "spironolactone bodies" (whorled, scroll-like, pink globule surrounded by a clear halo) are found adenomas from patients with hyperaldosteronism treated with spironolactone
Adenomas that produce sex hormones (virilization or feminization):
- Rare tumors that cause virilization in women and feminization in men
- Grossly, the tumors tend to have a mahogany grown cut surface
- Microscopically, the cells tend to resemble zona reticularis cells with eosinophilic, compact cytoplasm and are arranged in a solid pattern.
Note that adrenal adenomas secreting aldosterone causes 75% of primary aldosteronism, while adrenal adenomas secreting cortiosteroids causes only 15% of Cushing syndrome (the rest being a result of pituitary adenomas or ectopic ACTH production).4
Most are discovered incidentally on imaging. Prevalence increases with age, reported as ~7% in patients 70 years or older. There is no gender predilection.3
May clinically present with symptoms of Cushing syndrome, hyperaldosteronism or virilization/feminization depending on the type of hormone overproduced by adenoma.
Surgical excision. Tumor size is an important predictive factor. Most physicians advocate surgical excision for tumors greater than 6 cm due to significant cancer risk. Masses less than 3 cm can be monitored radiographically and biochemically. There is controversy in managing masses between 3 and 6 cm.
→Most (80%) of cortical adenomas are nonfunctioning (do not produce hormones).
→Functioning adenomas most commonly present with hyperaldosteronism and Cushing syndrome.
→Size is an important factor in determining treatment and cancer risk.
• Adrenal : Cortical Carcinoma
1 Kumar V, Abbas AK, Fausto N. Robbins and Cotran Pathologic Basis of Disease. 7th Ed. Philadelphia, PA: Elsevier; 2005: 1217.
2 Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 1100-3.
3 Griffing GT. Adrenal Adenoma: eMedicine (Last updated 8/19/09) Available at: emedicine.medscape.com/article/116587-overview
4 Thomspon LDR. Endocrine Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elsevier; 2006: 205-214.