
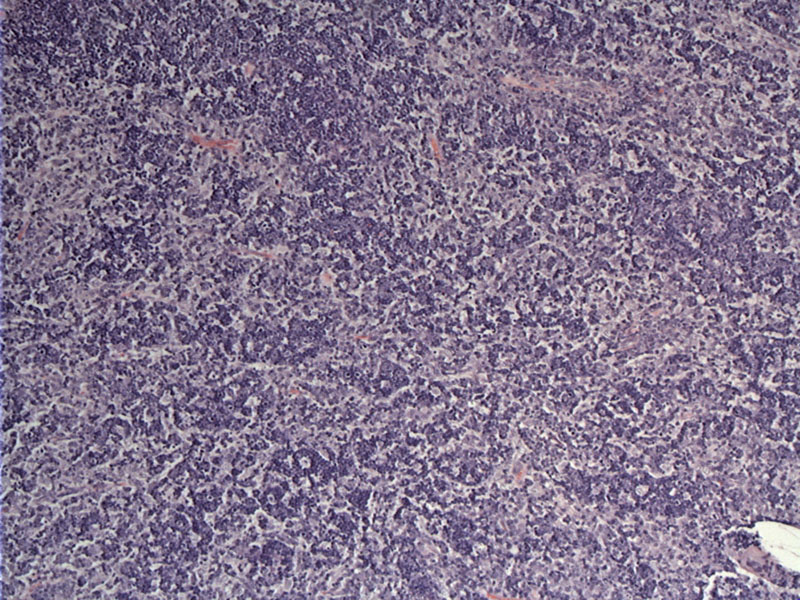
Case 1 - Neoplastic epithelial cells are enlarged with open chromatin pattern and form a delicate loose network. Lymphocytes are still numerous, but less so when compared to type B1.
The epithelial cells have open vesicular chromatin and nucleoli are visible, even at this low power.
The epithelial cells tend to line up next to fibrous septae as seen here. Type B2 thymomas are often lobulated.
At high power, you can appreciate the open chromatin, round nuclear contours and prominent nucleoli.
Case 2 - Another case demonstrates the presence of the pale interconnecting cords of epithelial cells admixed with lymphocytes.
The epithelial cells do have tendency to pallisade around perivascular spaces, although this is not very prominent here.
In type B2 thymoma, the neoplastic thymic epithelial cells are increased in number. They appear as scattered or aggregates of plump cells in a background population containing numerous lymphocytes. The epithelial cells are large, polygonal cells, with large vesicular nuclei and central prominent nucleoli. The epithelial cells have a tendency to palisade around vessels and fibrous septa. Dilated perivascular spaces are commonly found. These tumors are considered the equivalent of mixed lymphoepithelial thymoma in the traditional classification.
Compared to type B1, the lymphocytes are fewer in number and medullary differentiation is not present.
In about 20% of cases, there are epithelial-predominant type B3 areas and such tumors should be diagnosed as type B2/B3 thymomas (Fletcher).
Patients may present due to symptoms secondary to involvement of local structures or with an asymptomatic findings on chest xray. The most common presenting symptoms include dyspnea, chest pain, cough, superior vena cava syndrome (for higher stage disease), a paraneoplastic entity, and symptoms related to myasthenia gravis.
A combination of surgery, chemotherapy, and radiation may be used depending on stage. Complete surgical resection is always the goal.
Thymomas are typically slow-growing and spread by local extension. Metastases are usually confined to the pleura, pericardium, or diaphragm, and extrathoracic metastases are not typical. These tumors are also known to have a propensity for late recurrence despite even complete resection.
Stage is the single most important prognostic factor. Type A and AB thyomas tend to be stage I or stage II tumors. As you move from B1 to B3, there are more stage III and stage IV tumors.
About 10% of those with myasthenia gravis develop a thymoma
Type B2 thymoma appears morphologicaly similar to B1 -- small lymphocytes dominate the histology, but in B2, the relative proportion of epithelial cells is somewhat greater, and individual cells appear more prominent, showing larger nuclei and easily discernible nucleoli, relative to type B1
B2 is referred to as mixed lymphoepithelial thymoma and corresponds best to the pure cortical-type thymoma of the MH system
Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 1326.