
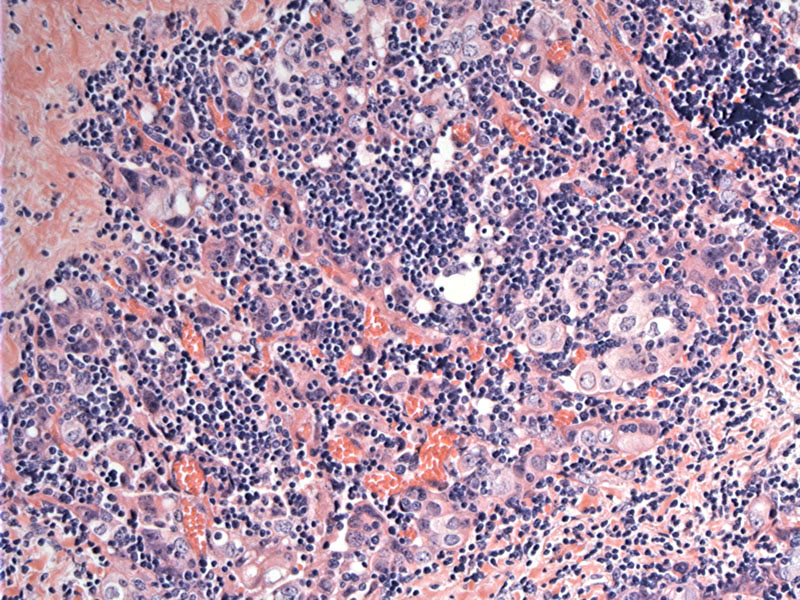
Anastomosing nests of neoplastic epithelial cells are intermingled with a lymphoplasmacytic infiltrate.
Broad cords of squamoid cells are intimately admixed with the lymphoid cells.
On higher power, you can appreciate the enlarged pleomorphic cells that are crowded and overlapping. Perhaps you can even distinguish between the lymphoid cells and plasma cells.
Marked pleomorphism is seen and the neoplastic cells have indistinct cytoplasmic borders. Lymphoepithelial-like carcinoma is essentially a poorly-differentiated squamous cell carcinoma with a lymphoplasmacytic infiltrate.
Thymic carcinomas come in a variety of histologic subtypes, the most common being squamous cell carcinoma which is further subclassified as well, moderately or poorly differentiated. Poorly-differentiated lesions are often associated with a lymphoplasmacytic infiltrate, and thus are often called "lymphoepithelial-like carcinoma".
Lymphoepithelial-like carcinoma is histologically identical to that seen in the nasopharynx. Histologically, a syncytial sheet of pleomorphic epithelial cells are admixed lymphocytes and plasma cells. There can be focal squamous differentiation in some instances. Approximately 50% of cases are positive for EBV antigens with the majority of cases arising in children and young adults (Fletcher). There is controversy regarding this association, however, as studies have not been consistent (Moran).
Resectability seems to be the only prognostic factor in thymic carcinoma overall. Preoperative evaluation to exclude unresectable Masaoka stage IVb disease is recommended and expect preoperative chemotherapy or chemoradiotherapy to improve the respectability.
• Cervix : Lymphoepithelial-like Carcinoma
Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 1331-2
Moran CA, Suster S. Thymic carcinoma: current concepts and histologic features. Hematol Oncol Clin North Am. 2008 Jun;22(3):393-407.
