
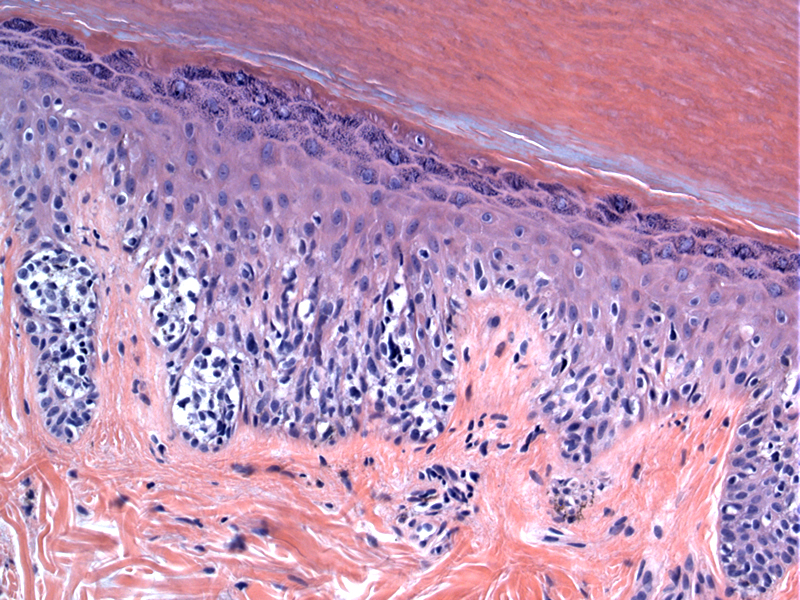
Overgrowth of atypical melanocytes at the dermal-epidermal junction is known as melanoma in situ. A few melanocytes may permeate superficial epidermal layers; involvement of cutaneous adnexal structures is common. Nuclear atypia is variable and may be subtle.
The atypical melanocytes are confluent along the dermal-epidermal junction with bridging of the rete pegs. Small nests may even be present.
Melan-A highlights the melanocytic proliferation. Sometimes this marker can be used to help evaluate the margins.
By definition, lentigo maligna occurs on chronically sun-damaged skin, with abundant solar elastosis in the superficial dermis. This is accompanised by epidermal atrophy, increased pigmentation in basal keratinocytes.
Lentigo maligna (LM) is defined as melanoma in situ of sun-exposed skin. If sun-exposure is not evident, i.e. solar elastosis is not identified, then the lesion is called simply melanoma in situ.
Histologically, atypical melanocytes line the basal epithelium, and can be found in the epidermis and exhibit pagetoid spread. There is no invasion into the dermis, however. Solar elastosis must be present in the dermis, by definition. The epidermis is often atrophic in LM.
Typically develops as a slowly enlarging pigmented macule on sun-damaged skin, usually on the head or neck, although any site with chronic exposure to UV radiation may be involved. The macule, or patch, may show asymmetry, an irregular peripheral border, and a variegated color. The in situ stage can last for a long time and in fact, only 5% of LM become invasive (Rapini).
Surgical options include simple excision and Mohs micrographic surgery; cryosurgery, radiotherapy, electrodessication and curettage, laser surgery, topical 5-fluorouracil, and azelaic acid.
Left untreated, some LM may continue to grow, resulting in dermal invasion and progression to lentigo maligna melanoma. Lesions have a tendency towards repeated recurrence following seemingly adequate treatment. Estimates of recurrence rates range from 20 to 100% at 5 years.
→Lentigo maligna is melanoma in situ in sun exposed skin. If there is solar elastosis, the entity is simply called melanoma in situ.
→If invasion is present, the term lentigo maligna melanoma is used.
Rapini RP.Practical Dermatopathology. Philadelphia, PA: Elsevier; 2005: 278.
Reed JA, Shea CR. Lentigo maligna: melanoma in situ on chronically sun-damaged skin. Arch Pathol Lab Med. 2011 Jul;135(7):838-41.