
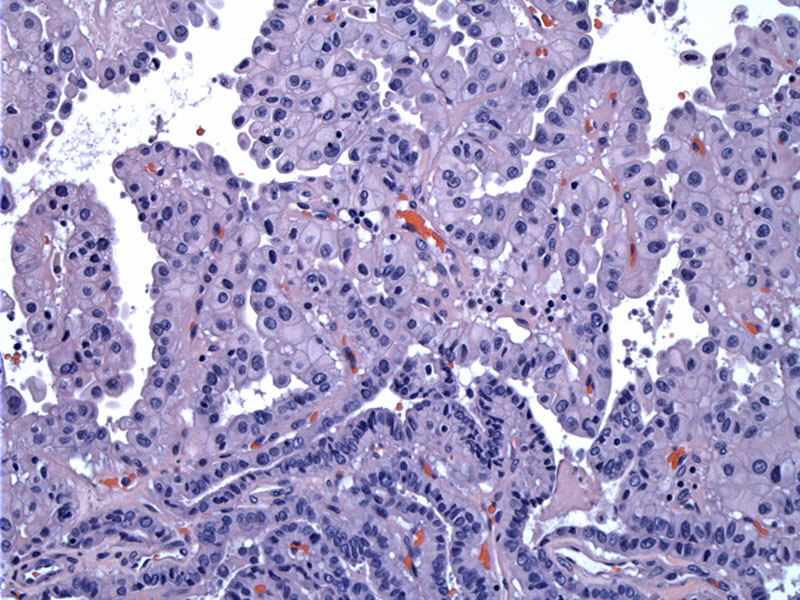
Conventional PTC is seen at the bottom with a transition to the oncocytic type. While these tumors can show various patterns, typically the predominant architecture is papillary as seen here.
Typical nuclear features of papillary carcinoma are prevalant. Nuclear inclusions are easily found (arrows).
Abundant densely eosoinophilic cytoplasm (oncocytic) is present. Numerous mitochondria occupy the cytoplasm as studied by electron microscopy.
An area with some follicle formation is also present.
Focal nuclear apical polarization (black arrow) is a recognized feature of this tumor.
Cervical lymph nodes are involved. Psammoma bodies are present in the metastatic area.
About 1/2 of these cases show BRAF mutation. A mutation in GRIM-19 gene has been found in a few tumors, a gene involved in mitochondrial metabolism and cell death. Other tumors show the RET/PTC gene rearrangement. About 1/3 of cases show a background of chronic lymphocytic thyroiditis (Hashimoto's).
In a study of 23 cases, interestingly, none of the cases presented as encapsulated tumors (Gross).
Given the higher incidence of local invasion and cervical lymph node involvement, more extensive surgery than classic papillary thyroid carcinoma may be required (Gross).
Although limited information is available due to the rarity of the tumor, it does not appear to behave aggressively (Berho)(Beckner).
• Thyroid : Papillary Carcinoma, Follicular Variant
• Thyroid : Papillary Carcinoma, Solid Variant
• Thyroid : Papillary Carcinoma, Tall Cell Variant
• Thyroid : Papillary Carcinoma, Warthin's Variant
• Thyroid : Papillary Thyroid Carcinoma, Cribriform-Morular Type
Gross M, et al. Clinicopathologic features and outcome of the oncocytic variant of papillary thyroid carcinoma. Ann Otol Rhinol Laryngol. 2009 May;118(5):374-81.
Berho M, Suster S. The oncocytic variant of papillary carcinoma of the thyroid: a clinicopathologic study of 15 cases. Hum Pathol. 1997 Jan;28(1):47-53.
Beckner ME, Heffess CS, Oertel JE. Oxyphilic papillary thyroid carcinomas. Am J Clin Pathol. 1995 Mar;103(3):280-7.